

Staffing Isn’t the Only Problem: Why Hospital Burnout Persists Even After Hiring Improves?
At 12:55, the clinic is still running. At 1:00, the next block begins anyway. Somewhere in between, a policy says there is a break, but the day does not.
Burnout does not always show up as a dramatic crisis. Sometimes it shows up as a hospital that keeps functioning, while recovery time quietly disappears, supervision load quietly grows, and the hardest decisions keep landing on the same few desks.
This MDForLives pulse looks at where hospital administrators and operations leaders say strain is coming from right now, what is driving exits, what is failing to move the needle, and which leadership decisions are most underestimated when burnout builds.
When people say “workforce strain,” what do they actually mean?

The first signal is still what most hospitals expect: 36% point to clinical or allied staff shortages as the biggest operational strain.
But the story changes in the very next line. 24% say the bigger problem is high turnover despite active hiring, and another 16% point to burnout-related productivity decline. Even when staffing improves on paper, the operation can still feel like it is running on soft ground, because continuity is not rebuilt at the same speed as headcount.
What this suggests is a shift in the nature of the problem: from “we are short” to “we are unstable.” Hiring helps, but it does not automatically restore rhythm, trust, or experience density across shifts.

“Leadership keeps counting hires, but the operational reality is continuity. We keep rebuilding teams instead of strengthening them.”
Maya R, Hospital Operations Director (MDForLives panelist, composite)
Why stability can feel “flat” even when hiring improves
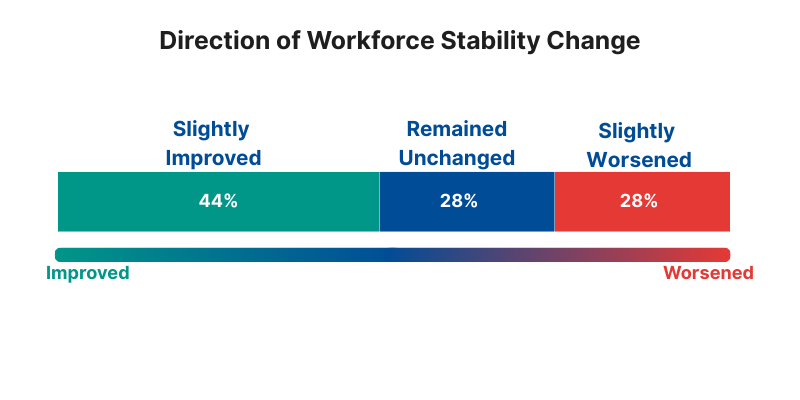
When asked about workforce stability over the past 12 months, the most common answer is not improvement or decline. It is “remained unchanged” at 28%.
At the same time, the organization is not uniformly stuck. A combined 44% describe stability as improved (slightly or significantly), while 28% describe it as worsened (slightly or significantly). That split is important because it hints at uneven recovery: some units stabilize while others remain in a loop of churn, strain, and catch-up.
That is how burnout persists in the middle. Not when the whole system collapses, but when the hardest areas never get back to baseline and the rest of the hospital keeps compensating.
The quiet retention problem: early exits that erase momentum
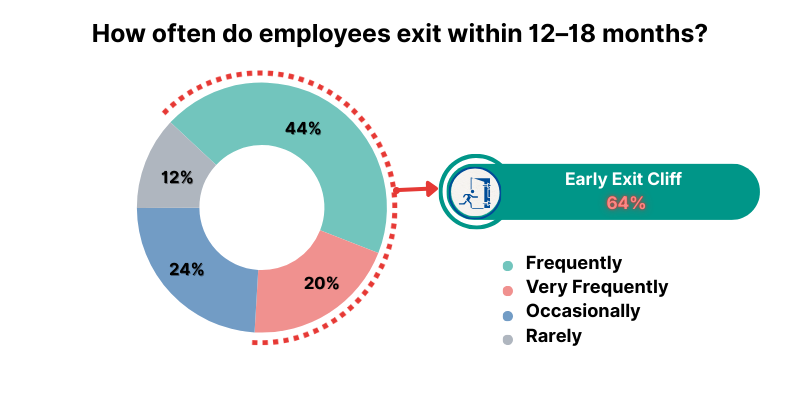
One of the strongest signals in this pulse is how often employees exit within the first 12–18 months.
A combined 64% say this happens frequently (44%) or very frequently (20%). In other words, even if recruiting improves, the organization can still lose the very time it needs to rebuild capability. Early exits pull senior staff into constant supervision, constant training, and constant rework. That is not just a retention metric. It is an operational drag.
When early exits become normal, “burnout” stops being an individual experience and becomes a property of the system: too much onboarding, too little recovery, and too many fragile handoffs.
What is driving turnover: money, or the design of the day?
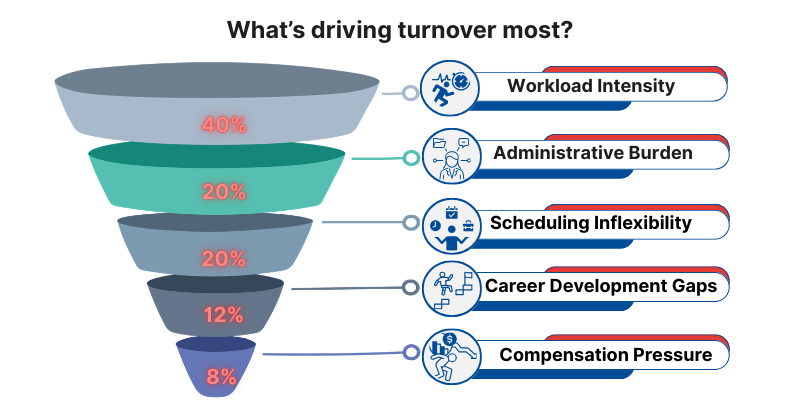
When hospital admins point to the strongest driver of turnover, the leading answer is not compensation. It is workload intensity at 40%.
Then come two forms of friction that staff feel daily: administrative burden (20%) and scheduling inflexibility (20%). Compensation pressure appears, but much lower at 8%.
This pattern reads like a work-design problem more than a motivation problem. People are not only leaving because they are unhappy. They are leaving because the work is structured in a way that does not recover.
It also explains why hiring alone can fail to change the lived experience. If workload intensity is the central driver, and scheduling plus admin friction reinforce it, the system can remain exhausting even with more bodies in the building.

“The handbook says there’s a break. The workflow says there isn’t. People learn very quickly what the system will not protect.”
Daniel K, Clinic Operations Manager (MDForLives panelist)
Burnout as a continuity risk, not a wellbeing topic
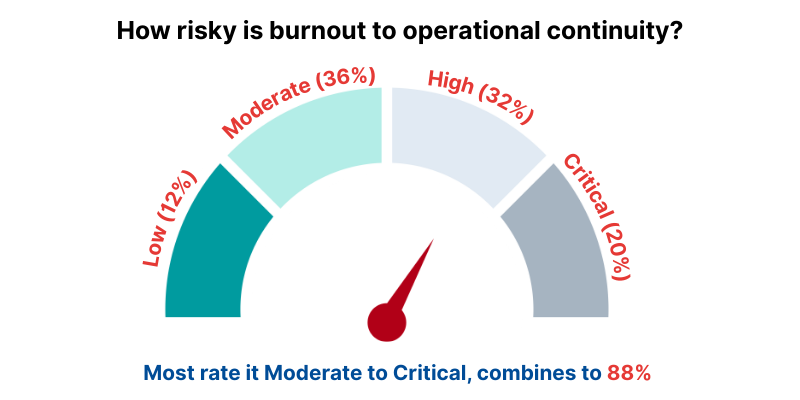
Burnout is not being dismissed as “soft.” Most respondents rate it as an operational risk: 36% moderate, 32% high, and 20% critical.
At the same time, views on staffing sustainability over the next 2–3 years are split in a way that should make leaders pause. 40% believe the model is sustainable without major change, while 32% believe it is unsustainable without intervention, and 28% say it is sustainable only with redesign.
That split often appears right before a tipping point. Not because people disagree on whether burnout exists, but because hospitals can keep functioning while silently spending workforce capacity faster than it is replenished.
What exhausts staff is not one constraint. It is a trio that feeds itself.
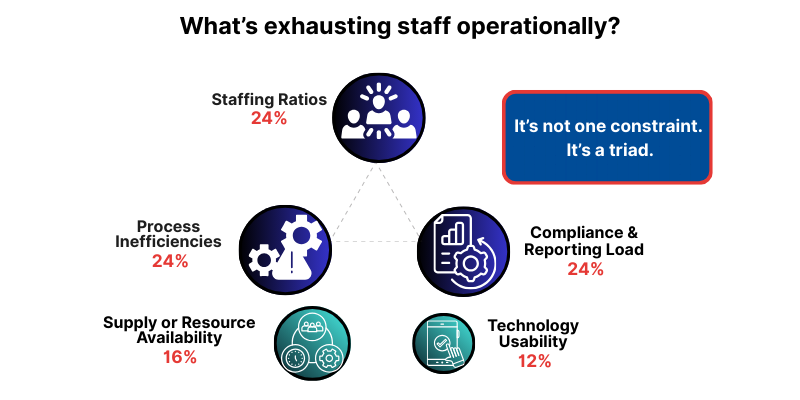
When admins describe what contributes most to staff exhaustion, three pressures tie at the top, each at 24%: compliance and reporting load, process inefficiencies, and staffing ratios.
That combination matters because it compounds. Staffing ratios tighten, which increases pressure and mistakes. Mistakes and variability increase reporting and
compliance load. Reporting load steals time, which makes process inefficiencies more punishing. Inefficiency then increases the staffing ratio pressure again.
Add in supply or resource availability at 16%, and technology usability at 12%, and you get a picture of exhaustion that is operational, cumulative, and rarely solved by a single initiative.
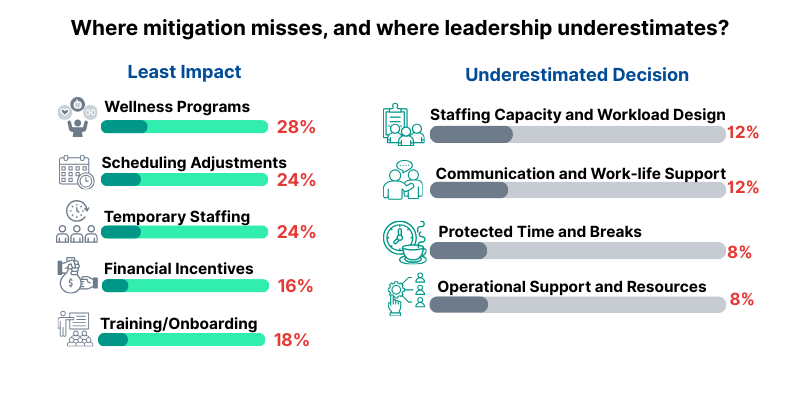
Why mitigation efforts fail to “land” even when they are well-intentioned
When asked which mitigation effort has delivered the least measurable impact, wellness programs lead at 28%. Scheduling adjustments and temporary staffing follow closely at 24% each.
That does not mean wellness is useless. It often means wellness is being asked to compensate for structural load. If the system keeps removing breaks, keeps adding reporting weight, and keeps running at the same pace under thinner staffing, wellness becomes a bandage placed over a design issue.
Even procurement and vendor dependency plays a role here, not as the main cause, but as an amplifier. Most see it as a smaller contributor, with 44% saying it contributes slightly and 24% moderately. “Slight” does not mean harmless when the impact is felt daily through tool sprawl, supply friction, and workflow interruptions.
The most underestimated decision is where accountability becomes emotional weight
The open ended question lands on one theme more than any other: 52% point to high-stakes clinical decisions and accountability as the leadership decision most underestimated in burnout.
This is where burnout stops being “fatigue.” It becomes moral load plus operational load at the same time. Decisions about prioritization, discharge timing, cross-border transfers, end-of-life pathways, and scarce resource allocation carry consequences that are subtle, ethically complex, and emotionally charged. When those decisions are made under pressure, with thin recovery time, the workforce absorbs the moral residue of the system.
Other themes reinforce the same story: workload design and staffing capacity (12%), communication and work-life support (12%), and then the practical basics that staff feel in their bodies, like protected time and real breaks.
Wrap up
If burnout was only about shortages, hiring would solve it.
This pulse points to something more operational: burnout persists when continuity is fragile, early exits are common, and workload intensity is reinforced by admin friction and thin recovery time.
That is why the most underestimated leadership decision is not a wellness budget. It is the decision to keep the system running at the same speed, even when the workforce can no longer recover at that speed.
The real question is not “Can we hire?” It is: Can we redesign work before burnout redesigns the workforce for us?
Frequently Asked Question
Why does burnout persist even after hiring improves?
Because hiring can increase headcount without restoring continuity. High turnover, early exits, and daily friction can keep workload intensity high.
What is the strongest driver of turnover in this pulse?
Workload intensity leads, followed by administrative burden and scheduling inflexibility.
Why do wellness programs often feel ineffective?
Wellness cannot offset structural load if recovery time, workflow design, and reporting burden remain unchanged.
What leadership decision is most underestimated?
Many respondents point to high-stakes decisions and accountability, where operational choices carry ethical and emotional weight.
Hope this insight added value.
Participate in the survey below and add your voice to the conversation.
About Author : MDForlives
MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.



