
Neurologist Insights on Stroke Care Gaps: Timing, Uncertainty & Systems
When the clock is running and onset is uncertain, what do you defend: the guideline, or the patient?
Not in the protocols.
Not in the science.
But in the minutes around them.
Unclear onset.
Borderline deficits.
Transfers that stretch the clock.
And what happens after discharge, when structured plans meet real life.
Stroke care is built on strong evidence. Guidelines are clear. Pathways are widely taught. Yet daily practice rarely unfolds in clean steps. Decisions slow when information is incomplete, when timing is uncertain, and when care depends on coordination beyond a single team or site.
To understand where stroke care most often stalls, neurologists across the USA, UK, Canada, France, Germany, and Italy were asked about their day-to-day decisions.
What emerged was not confusion about treatment.
It was a pattern.
And patterns are where practice turns into insight.
Why is the thrombolysis window still lost before hospital arrival?
By the time many stroke patients reach the hospital, the most important decision has already been made.
Not by a clinician.
By time.
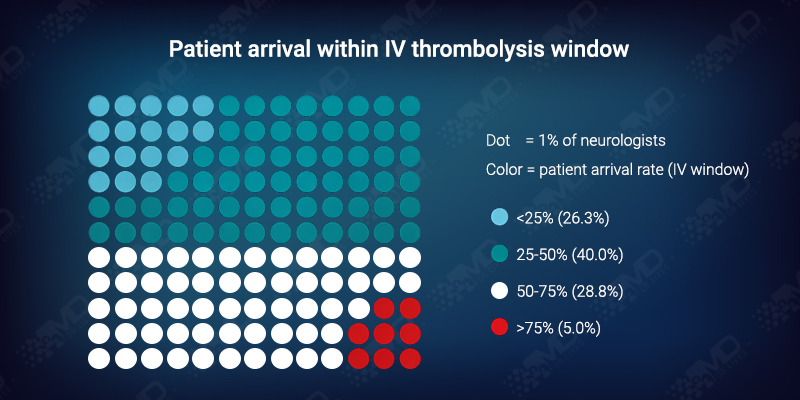
Only a small minority report that most suspected ischemic stroke patients arrive within the IV thrombolysis window.
This distribution suggests that pre-hospital timing is a major limiter, even before in-hospital efficiency comes into play. Late arrival and unclear or wake-up onset appear to dominate eligibility loss upstream.
This means even the fastest door-to-needle workflow cannot rescue a patient who arrives too late.

“If the onset is unclear, everything else becomes secondary. You are no longer asking whether the patient is eligible, but whether the risk is still acceptable.”
Dr. Luca Moretti, Consultant, Italy
Pre-hospital delay is rarely a single failure. Neurologists describe a familiar cluster: delayed symptom recognition, delayed EMS activation, wake-up stroke ambiguity, and triage to non-stroke centers due to geography or access.
Why this matters: Once eligibility is lost upstream, no amount of excellence downstream can undo it.
Are borderline cases the norm in daily stroke care?
Borderline cases are not exceptions in stroke care.
They are the operating environment.
Neurologists use the term “borderline” to describe presentations that sit just outside clean thresholds: unclear onset, mild but potentially disabling deficits, anticoagulated patients, rapidly improving symptoms, and posterior circulation ambiguity.
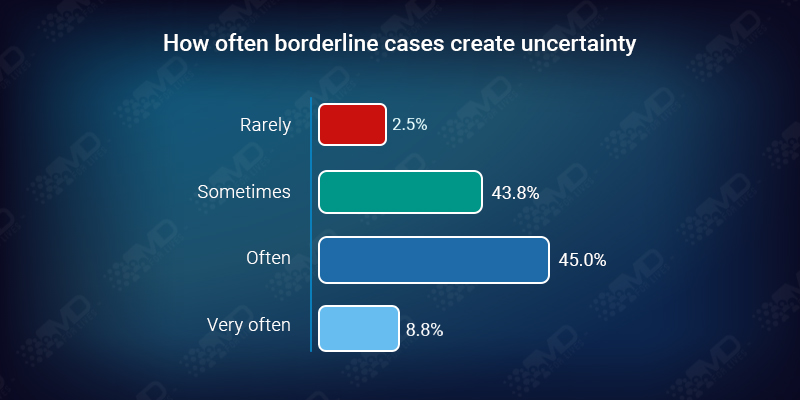
Nearly all neurologists encounter these cases regularly. They shape daily decision-making far more than textbook presentations.
Guidelines handle clean cases well. Real-world practice is shaped by situations where timing, information, or risk tolerance fall into a gray zone.
These cases consume disproportionate time because the risk is not only clinical, but also defensibility under uncertainty.
Guidelines are effective for deciding what to do.
They are less helpful for deciding what can be defended when the clock is running and information is incomplete.
When Guidelines Hold and Judgment Stretches
Stroke decisions are rarely purely protocol-driven.
Even in guideline-led environments, neurologists rely on judgment when cases sit at the edges of eligibility. This is not variation in standards. It is conditional reliance.
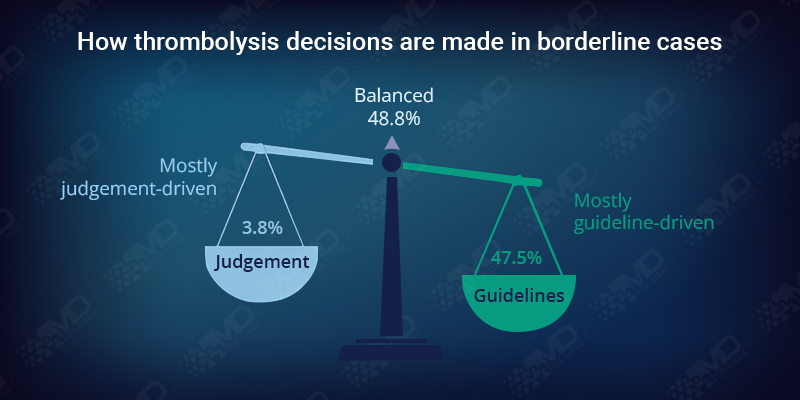
In these moments, judgment performs specific work. Interpreting functional disability. Weighing hemorrhagic risk. Resolving imaging ambiguity. Considering medico-legal defensibility when evidence does not map cleanly to the patient in front of them.
The guideline is the anchor.
The edge case is where the real work happens.
Protocols anchor decisions.
They do not replace reasoning when certainty breaks down.
Why Thrombectomy Still Slows Down?
When thrombectomy is delayed, neurologists rarely point to uncertainty about eligibility.
They point to the system.

“With thrombectomy, the question is often not eligibility. It is whether the patient will still be in window once transfer is complete.”
Dr. Sarah Whitfield, Consultant Neurologist, United Kingdom
Inter-hospital transfers and limited access to thrombectomy-capable centers dominate the delay landscape. Together, these system-level factors outweigh imaging delays, staffing constraints, and patient-related causes.

A useful contrast emerges from neurologist experience.
Thrombolysis is a single-site sprint.
Thrombectomy is a network relay.
Even when eligibility is clear, treatment speed depends on referral pathways, transport logistics, and access to intervention slots.
Why this matters: in thrombectomy, speed is shaped by network architecture, not individual clinician performance.
When Imaging Becomes the Bottleneck
For about half of neurologists, imaging rarely delays acute stroke decisions.
For the rest, delays cluster around advanced imaging and interpretation.
Baseline CT access is generally reliable. Decision-making slows when additional certainty is required. Wake-up stroke. Extended windows. Mild deficits with uncertainty. Suspected posterior circulation events.

In many cases, the friction appears less about scanner availability and more about the need for added certainty and interpretation.
The scan is available.
The decision is harder.
Why Hemorrhagic Outcomes Still Vary?
Hemorrhagic stroke outcomes remain heavily dependent on early presentation and institutional readiness.
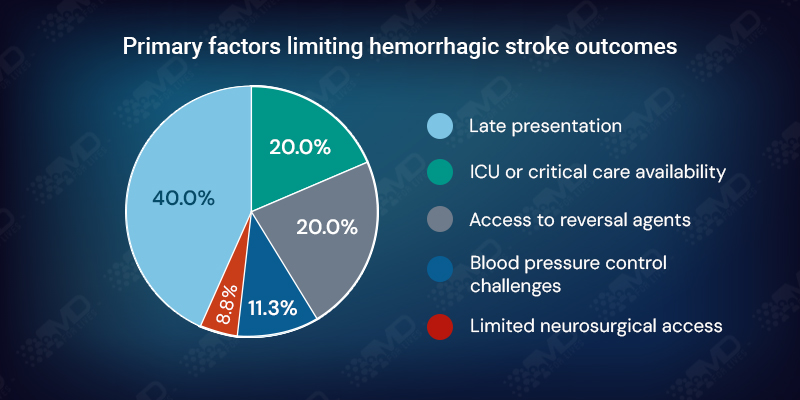
Late arrival is cited most often, followed by ICU or critical care availability and access to reversal agents. Neurologists also point to variability in neurosurgical access, reversal workflows, blood pressure protocol consistency, and the timing of goals-of-care discussions.
Hemorrhage outcomes swing with readiness, not just decisions.
Where Prevention Breaks After Discharge
Most neurologists agree on one point.
Recurrent stroke is often preventable.
Breakdowns are most commonly attributed to what happens after discharge, not during acute care.
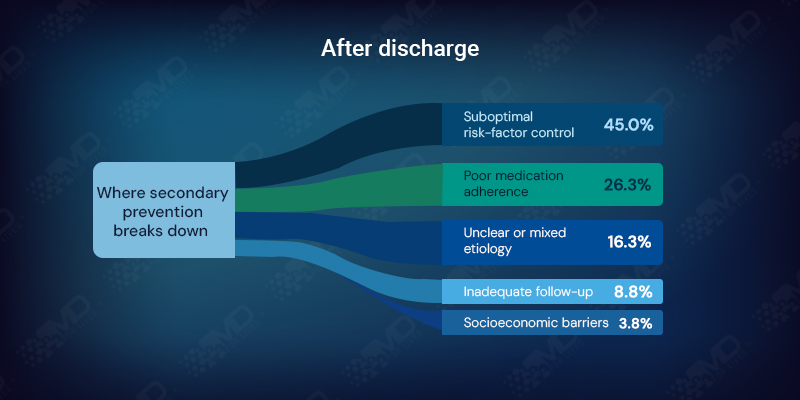
Gaps cluster around risk-factor control and medication adherence, followed by unclear or mixed etiology and gaps in follow-up.
Acute stroke care is a managed pathway.
Secondary prevention is a handoff to the real world.
Where do guidelines fall short in practice?
Guidelines work best when timing is clear and systems function as designed.
They offer less support when uncertainty and coordination dominate.

Neurologists consistently point to three gaps: ambiguity at presentation, network friction across sites, and post-discharge continuity of care.
Very few see the core evidence for thrombolysis as the weak point.
The challenge is execution under constraint.
Closing Perspective
Across the stroke pathway, the same pattern repeats.
Time pressure.
Uncertainty.
System design.
Neurologists are not questioning the science.
They are defining the conditions under which it can work.
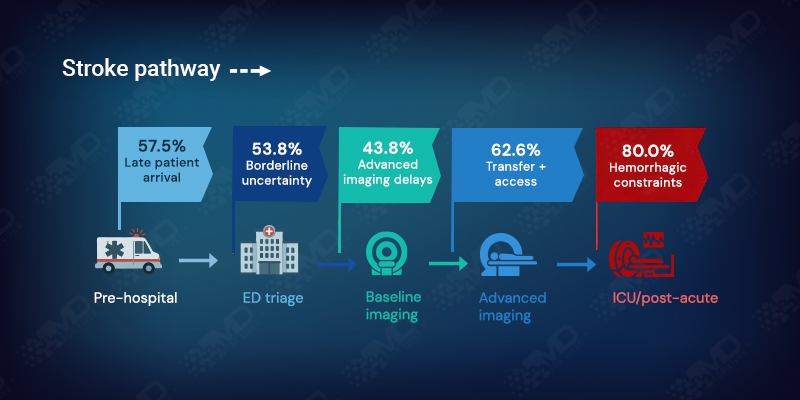
Stroke care fails less in the science, and more in the seams between steps.
Taken together, the data points to a clear conclusion: stroke outcomes improve fastest when systems are built for edge cases, not just ideal ones.
If improvement levers exist, they are increasingly clear. Earlier recognition and smarter triage before arrival. Clearer pathways for borderline cases inside hospitals. Stronger ownership and follow-up after discharge.
Frequently Asked Questions
Why do so many stroke patients miss the thrombolysis window?
Most eligibility loss happens before hospital arrival. Late presentation, unclear or wake-up onset, delayed symptom recognition, and EMS routing reduce treatment opportunity before in-hospital care begins.
What do neurologists mean by “borderline” stroke cases?
These are presentations that fall outside clean guideline thresholds, such as unclear onset, mild but disabling deficits, anticoagulated patients, rapidly improving symptoms, and posterior circulation strokes.
Why is thrombectomy still delayed even when eligibility is clear?
Delays are mainly system-driven. Inter-hospital transfers, access to thrombectomy-capable centers, and network design influence speed more than individual clinician decisions.
When does imaging become a bottleneck in stroke care?
Imaging slows decisions when added certainty is required, including wake-up stroke, extended time windows, and suspected posterior circulation events.
Where does secondary stroke prevention most often break down?
After discharge. Gaps in risk-factor control, medication adherence, etiology clarity, and follow-up continuity weaken prevention outside structured inpatient pathways.
Hope this insight added value.
Participate in the survey below and add your voice to the conversation.
About Author : MDForlives
MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.


