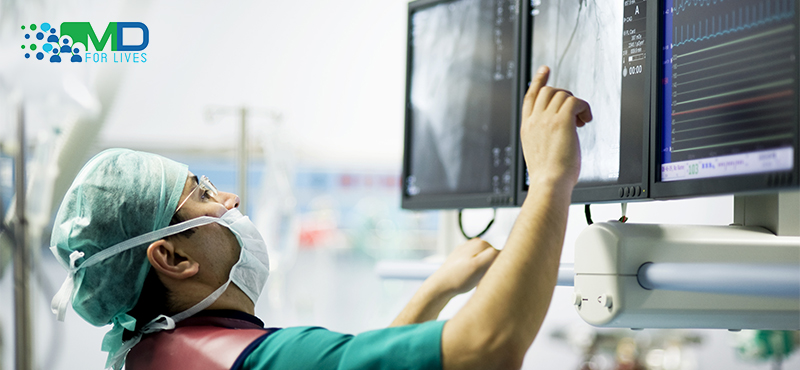
Complications from cardiac surgery remain a critical determinant of postoperative outcomes, influencing recovery timelines, hospital stay, and long-term survival. Understanding risk patterns, early detection, and management strategies is essential for improving patient safety and clinical results.
Overview of Cardiac Surgery & Risk
Cardiac surgery includes procedures such as coronary artery bypass grafting, valve repair or replacement, and congenital defect correction. These interventions address life-threatening conditions but involve complex physiological stress.
Risk is influenced by patient health status, surgical complexity, and perioperative care. Even with advancements, complications remain a measurable concern.
Why Cardiac Surgery Complications Matter
Postoperative complications directly affect both short-term recovery and long-term outcomes.
- Increased length of hospital stay
- Higher readmission rates
- Greater healthcare costs
- Reduced quality of life
Managing these complications is central to improving overall surgical success.
Cardiac Surgery Complications Classifications
Complications can be grouped based on clinical presentation:
| Category | Examples |
| Cardiac | Arrhythmias, myocardial dysfunction |
| Pulmonary | Respiratory failure, pneumonia |
| Neurological | Stroke, cognitive dysfunction |
| Renal | Acute kidney injury |
| Infectious | Surgical site infections |
This classification supports structured monitoring and intervention.
Mechanisms and Definitions of Key Complications
Each complication arises from specific physiological disruptions:
- Arrhythmias: Electrical instability following surgery
- Acute kidney injury: Reduced renal perfusion during or after surgery
- Respiratory complications: Impaired lung function due to anesthesia and immobility
- Infections: Exposure during surgical procedures
Understanding mechanisms supports targeted prevention.
Risk Factors and Predictors
Risk varies based on patient and procedural variables:
- Advanced age
- Pre-existing cardiovascular disease
- Diabetes or renal impairment
- Prolonged surgery duration
- Emergency procedures
Risk stratification tools are often used to guide clinical decisions.
Postoperative Outcomes: Observations
Clinical observations show that complications often occur within the early postoperative period. Continuous monitoring during this phase is essential.
Patterns include:
- Early onset arrhythmias
- Gradual respiratory compromise
- Delayed infections
These trends inform surveillance strategies.
Pathophysiology Insight – Why It Happens?
Surgical intervention triggers systemic responses:
- Inflammatory activation
- Hemodynamic fluctuations
- Tissue injury and repair processes
These responses can disrupt organ function, leading to complications if not managed effectively.
Clinical Monitoring and Early Detection Strategies
Early detection improves outcomes:
- Continuous cardiac monitoring
- Regular laboratory assessments
- Imaging where required
- Structured postoperative checklists
Timely identification allows prompt intervention.
Management Approaches for Complications
Management depends on complication type:
- Antiarrhythmic therapy for rhythm disturbances
- Ventilatory support for respiratory issues
- Renal support in cases of kidney injury
- Antibiotics for infections
Treatment is often multidisciplinary and tailored to patient condition.
Cardiac Surgery Complications Prevention
Preventive strategies focus on reducing risk before and after surgery:
- Preoperative optimization of patient health
- Standardized surgical protocols
- Infection control measures
- Early mobilization post-surgery
Prevention reduces both incidence and severity of complications.
Impact on Long-Term Outcomes
Complications influence long-term recovery and survival.
- Delayed functional recovery
- Increased risk of chronic conditions
- Reduced overall survival in severe cases
Effective management improves long-term prognosis.
Role of the Multidisciplinary Team in Managing Complications
Care involves collaboration between:
- Cardiac surgeons
- Cardiologists
- Intensive care specialists
- Nursing teams
This coordinated approach ensures comprehensive management.
Clinical Guidelines, Documentation, and Quality Metrics
Clinical guidelines standardize care and improve outcomes.
- Protocol-driven management
- Documentation of complications
- Monitoring quality indicators
These practices support continuous improvement in care delivery.
Case Studies on Cardiac Surgery Complications
Clinical case reviews highlight variability in complication patterns. Patients with similar procedures may experience different outcomes based on risk factors and response to treatment.
Case-based insights help refine clinical strategies and improve predictive models.
Conclusion
Complications from cardiac surgery are influenced by multiple factors spanning patient condition, surgical complexity, and postoperative care. Advances in monitoring, prevention, and multidisciplinary management continue to improve outcomes, though vigilance remains essential.
Explore more evidence-led healthcare insights and global perspectives: MDForLives
Frequently Asked Questions
What is the most common cardiac complication after cardiac surgery?
Postoperative arrhythmias, particularly atrial fibrillation, are among the most frequently observed complications.
Which patients are at highest risk for developing postoperative arrhythmias?
Older patients and those with pre-existing cardiac conditions are at higher risk.
When should patients be referred for cardiac rehabilitation after complications?
Referral is typically recommended once the patient is clinically stable and able to participate in structured recovery programs.
Can cardiac complications be completely prevented?
While risk can be reduced through preventive strategies, complications cannot be entirely eliminated.

MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.