Across healthcare practice and patient-reported experiences, stress-related symptoms are increasingly reflecting autonomic imbalance rather than isolated psychological causes. Clinicians frequently encounter individuals who continue to experience physiological stress responses long after an identifiable stressor has passed.
Rather than resolving once a situation ends, stress often persists in the body. It manifests through disrupted sleep, gastrointestinal discomfort, cardiovascular symptoms, emotional dysregulation, and fatigue. This pattern suggests that for many individuals, stress is not simply a mental state but a physiological condition maintained by the nervous system.
The parasympathetic nervous system plays a central role in restoring balance after stress. Understanding how it functions and how it can be intentionally activated offers a biologically grounded framework for reducing stress that goes beyond cognitive coping alone.
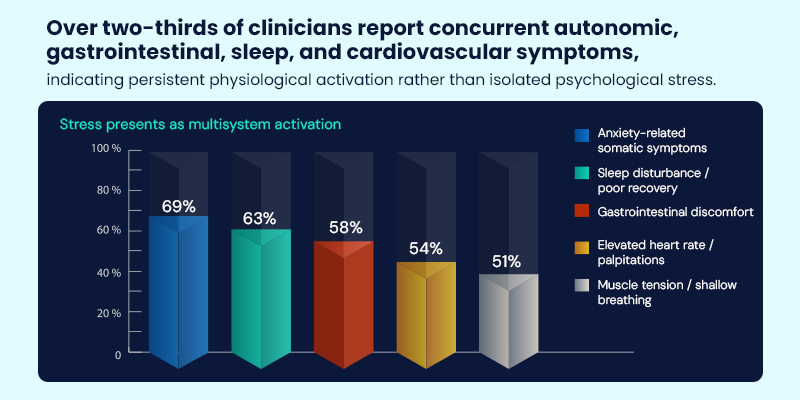
Clinician observations indicate that stress-related presentations rarely involve a single symptom. Instead, most patients exhibit overlapping autonomic, sleep, gastrointestinal, and cardiovascular manifestations. This points to persistent physiological activation rather than isolated psychological distress.
Key Takeaways
- Chronic stress often reflects autonomic imbalance, not purely emotional strain
- Stress symptoms commonly overlap across multiple body systems
- Addressing physiology can make emotional regulation more achievable
Why Stress Persists Beyond the Trigger?
Many individuals understand intellectually that a threat has passed, yet their bodies continue to respond as if danger remains. Clinicians consistently report that this disconnect between cognition and physiology is one of the most challenging aspects of stress-related care.
Traditional approaches often emphasize reframing thoughts, reducing worry, or changing perspective. While these strategies can be helpful, they frequently fall short when the nervous system remains physiologically activated.
Across real-world practice, clinicians consistently observe that cognitive strategies alone are insufficient when physiological stress responses remain elevated.
Stress becomes more responsive to intervention when bodily signals such as breathing patterns, heart rate, muscle tone, and sensory input are intentionally regulated. When these physiological cues shift, emotional and cognitive regulation often follow more naturally.
Clinicians report that meaningful emotional regulation typically follows successful physiological calming. This reinforces a body-first, mind-follows pattern in stress recovery.
What is the Parasympathetic Nervous System?
The parasympathetic nervous system (PNS) is responsible for conserving energy and supporting recovery during periods of rest. It counterbalances the sympathetic nervous system, which governs the body’s acute stress response.
Together, these systems regulate involuntary processes such as heart rate, digestion, respiration, and blood pressure. In both clinical and everyday contexts, parasympathetic activity determines how quickly the body recovers after stress exposure.
What Does the Parasympathetic Nervous System Do?
When parasympathetic activity increases, a coordinated calming response occurs:
- Heart rate slows
- Blood pressure decreases
- Digestive function improves
- Emotional regulation stabilizes
Chronic stress, particularly prolonged vigilance or fear-based rumination, can suppress parasympathetic tone. As a result, stress responses may persist even in the absence of immediate threat.
Where is the Parasympathetic Nervous System Located?
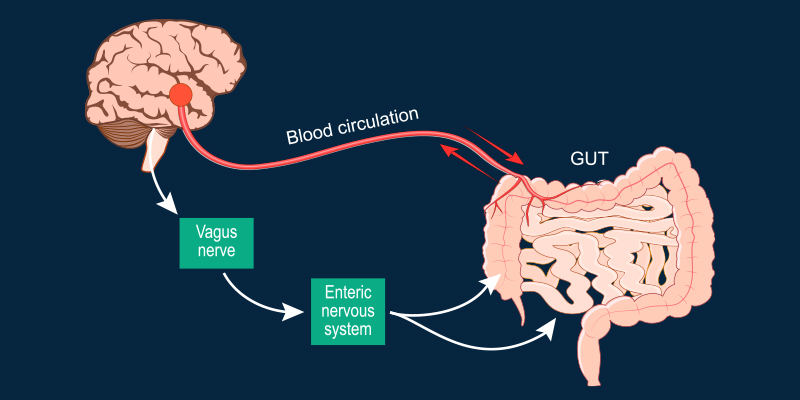
The parasympathetic nervous system originates primarily from the brainstem and sacral spinal cord. Its most influential pathway is the vagus nerve, which connects the brain to key organs including the heart, lungs, and gastrointestinal tract.
Ongoing neuroscience research continues to refine understanding of autonomic regulation. This work provides context for clinical patterns observed in stress, recovery, and resilience, without implying direct causality in individual outcomes.
Conditions Commonly Associated With Reduced Parasympathetic Activity
Reduced parasympathetic tone is commonly observed across a range of conditions, including:
- Chronic stress and burnout
- Anxiety and mood disorders
- Sleep disturbances
- Cardiovascular dysregulation
- Functional gastrointestinal symptoms
Across these presentations, autonomic imbalance often appears as a shared underlying mechanism rather than a secondary or incidental feature.
How Stress Reduction Works in Practice?
Effective stress reduction often begins with signaling safety to the nervous system. Rather than attempting to suppress symptoms cognitively, parasympathetic activation shifts bodily responses first. This creates the conditions for emotional and mental calm to emerge.
Simple and repeatable physiological interventions are often more sustainable than complex mental techniques, particularly when stress symptoms are persistent or multisystem.
Techniques to Stimulate the Parasympathetic Nervous System
Real-world clinical feedback consistently favors approaches that directly engage physiology rather than relying on cognition alone.
Real-world insight
In everyday practice, clinicians most often observe sustained stress improvement when interventions directly engage physiology. Body-based or multimodal approaches consistently outperform cognitive-only strategies.
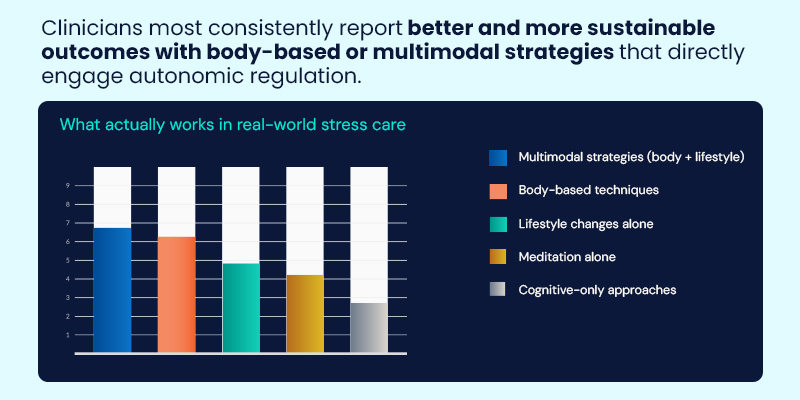
Commonly used techniques include:
1. Widening visual focus Stress narrows visual attention. Softening gaze and expanding peripheral awareness can reduce sympathetic arousal.
2. Slow breathing with longer exhales Breathing patterns with extended exhalation are among the most effective ways to increase parasympathetic activity.
3. Physiological sigh Two quick nasal inhales followed by a long exhale can rapidly reduce physiological arousal.
4. Meditation and mindfulness Practices emphasizing bodily awareness rather than cognitive effort alone are more likely to support parasympathetic engagement.
5. Postural and sensory regulation Changes in posture, muscle tension, and sensory input can meaningfully influence autonomic signaling.
Speed Matters in Stress Regulation
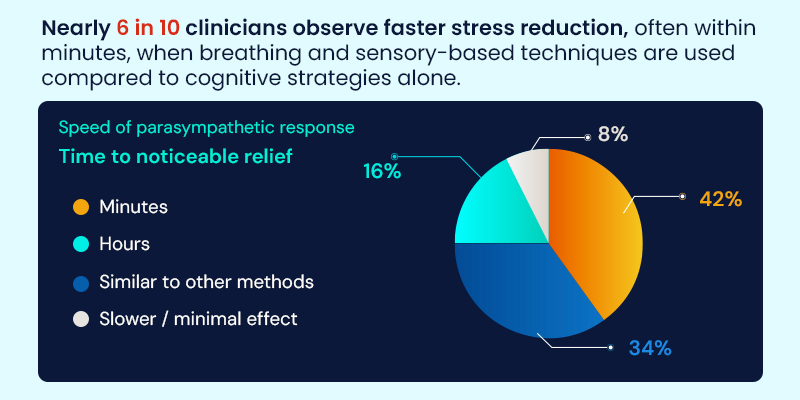
One of the most consistent observations across real-world clinical feedback is speed of response. Techniques that activate the parasympathetic nervous system are often associated with noticeably faster calming effects compared to cognitive strategies alone.
This immediacy can play a critical role in adherence, confidence, and sustained use, particularly for individuals who feel overwhelmed by prolonged stress symptoms.
Real-world insight
Speed emerges as a defining advantage of parasympathetic-focused techniques. Clinicians frequently observe calming effects much sooner than with cognitive approaches alone.
Key Takeaways
- Body-based and multimodal strategies consistently outperform cognitive approaches alone
- Parasympathetic activation is often associated with faster stress reduction
- Speed and physiological engagement matter for sustained regulation
Conclusion: Why Parasympathetic Regulation Matters
The parasympathetic nervous system is central to stress recovery, emotional resilience, and long-term health. Intentional activation through simple physiological techniques offers a practical and science-aligned approach to managing chronic stress without relying solely on cognitive effort.
What real-world insight adds is context. It shows how stress regulation actually unfolds outside controlled environments, where symptom overlap, time constraints, and adherence shape outcomes more than protocols alone.
Platforms like MDForLives help surface these real-world patterns by capturing clinician and patient perspectives across conditions and settings. This bridges biomedical understanding with lived healthcare experience.
Understanding stress regulation in real-world settings requires insight beyond controlled studies. MDForLives enables the collection of clinician and patient perspectives that inform how physiological stress responses are recognized, managed, and addressed in everyday care.
Frequently Asked Questions (FAQs)
What is the parasympathetic nervous system and why does it matter for stress?
The parasympathetic nervous system controls rest, recovery, and calming functions in the body. It reduces stress by slowing heart rate, supporting digestion, and helping the nervous system return to balance after stress has passed.
How does activating the parasympathetic nervous system reduce stress?
Activating the parasympathetic nervous system signals safety to the brain through slower breathing, reduced heart rate, and relaxed muscle tone. These physiological changes quiet the body’s stress response, allowing emotional and mental tension to settle naturally.
What are the most effective ways to stimulate the parasympathetic nervous system?
The most effective methods include slow breathing with longer exhales, meditation or mindfulness, widening visual focus, yawning, and simple breathwork techniques such as the physiological sigh. These approaches directly influence nervous system regulation rather than relying on cognitive effort alone.

MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.