

Diabetes Tech Helps, Yet Mental Load Stays High
Nothing went wrong today.
No emergency. No severe low. No scary spike.
And yet you end the day tired.
Not from a single crisis, but from the accumulation of tiny decisions: reading trends, reacting to alerts, predicting meals, correcting, waiting, checking again.
That is the contradiction in modern diabetes care. Tools have improved. Control has improved. But the mental load often has not.
In this MDForLives pulse survey of people living with diabetes across North America with additional Western Europe responses, 51.5% point to mental and emotional fatigue as the biggest remaining burden.
Visibility is up.
Cognitive load is not reliably down.
Why does the day still feel long?
Better monitoring shifts diabetes from occasional checking to continuous supervision, and supervision still demands attention.

Most respondents use CGM-based setups: 63.6% use CGM with insulin therapy, while 12.1% rely on fingerstick testing alone.
That shift reduces blind spots. But it also changes the shape of the day. Diabetes becomes less about moments of measurement and more about ongoing interpretation. You do not just check. You watch, anticipate, and adjust.
Key inference: Technology can make management safer while making diabetes more mentally present.
What relief does CGM really give?
CGM helps most by reducing uncertainty and fear, more than by removing decision-making.
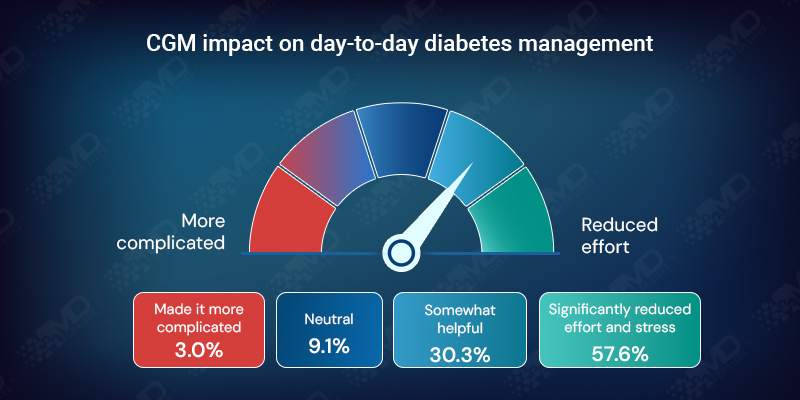
A majority report improvement: 57.6% say CGM significantly reduced effort and stress, and 30.3% say it was somewhat helpful.
Where the biggest relief shows up is also revealing. The most reduced challenge is fear of sudden highs or lows (33.3%), followed by night-time monitoring (24.2%).
Daytime management still runs on the same loop: interpret, decide, correct, re-check. The work becomes more informed, not absent.
Key inference: CGM often removes surprise, but it does not remove responsibility.
Why does accuracy matter most?
When people choose what they value most in CGM, accuracy leads because it determines whether data calms you or makes you second-guess yourself.

Accuracy and reliability (39.4%) outrank alerts (24.2%) and ease of use (18.2%).
False highs and false lows do not just create clinical risk. They create mental loops: should I correct, should I wait, should I double-check, should I trust my body or the sensor?
Key inference: Accuracy reduces second-guessing, and second-guessing is a major driver of fatigue.
Is automation offloading decisions?
It depends on whether the tool truly takes action, or only adds information that still needs supervision.
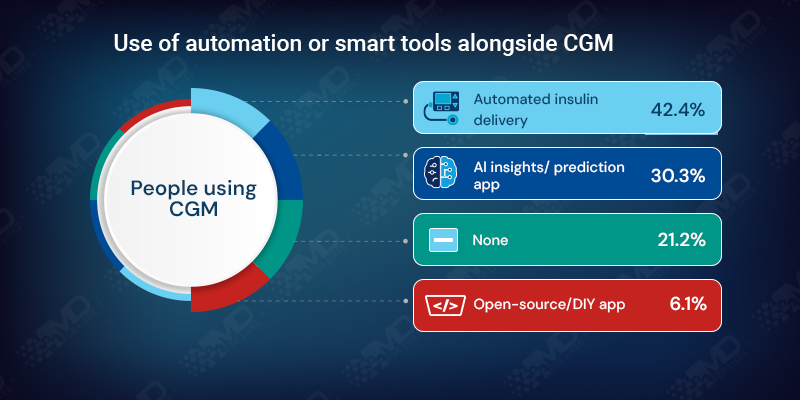
42.4% use automated insulin delivery, 30.3% use prediction or insight apps, and 21.2% use none.
Automation can remove decisions. Decision-support can add a new layer: more prompts, more interpretation, more “should I follow this?” moments.
Key inference: Some tools reduce thinking. Others turn diabetes into a supervision job.

“I’m safer with automation, but I still feel like the final safety officer. The thinking never fully leaves me.”
Daniel, 41, using automated insulin delivery
Do alerts bring peace of mind or more noise?
Most people rate predictive alerts as helpful, but helpfulness is not the same as rest.

60.6% say very helpful and 30.3% say somewhat helpful.
Alerts reduce surprise, but they also demand attention. They replace uncertainty with interruption, and interruption has a cognitive cost.
Key inference: An alert can prevent a spike while still adding mental load.
Why does fatigue still lead?
Because control often rises by increasing attention, not by reducing it.
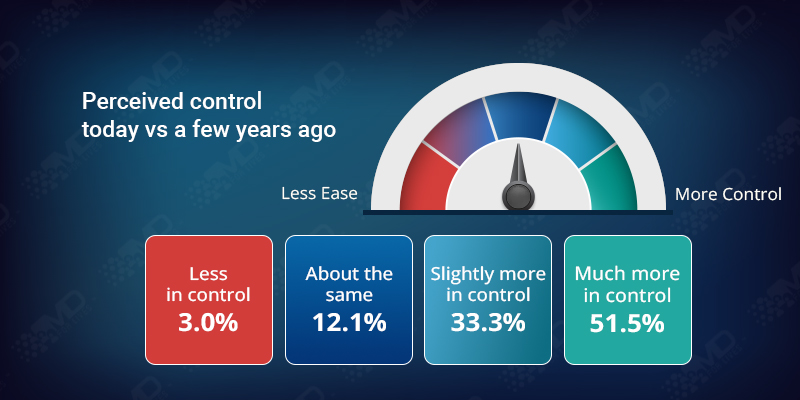
51.5% feel much more in control, and 33.3% feel slightly more in control.
Now compare that with what still weighs most.

Mental and emotional fatigue leads at 51.5%, well ahead of cost and access (18.2%) and data overload (15.2%).
Those two truths coexist because control is being earned through micro-decisions. Even a “good day” still requires constant judgment.
Key inference: Better control can come with a higher cognitive price when decision-making stays constant.
What has tech reduced most?
Technology helps most when it replaces vigilance, especially around safety and sleep.
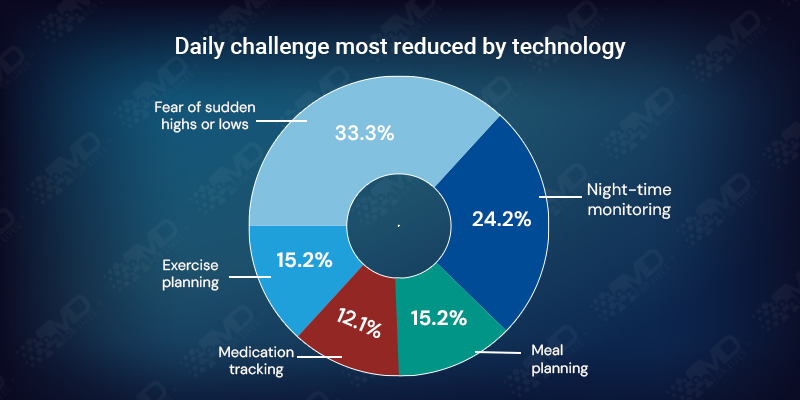
Top relief areas are fear of sudden highs or lows (33.3%) and night-time monitoring (24.2%). Relief is lower for meal and exercise planning (15.2% each), where interpretation and planning still dominate.
Key inference: Quiet monitoring reduces fear. Planning-heavy tasks still consume bandwidth.

“Night-time feels less scary now, but meals and corrections still feel like a full-time mental task.”
Sofia, 29, living with diabetes
Do food strategies lighten it?
Meal sequencing and personalized nutrition help many, but they do not always reduce effort because they can add planning and attention.

33.3% say yes, a lot and 42.4% say somewhat. 21.2% have not tried.
That pattern fits the broader theme: better outcomes do not always mean a lighter day.
Key inference: Strategies can improve numbers while still adding cognitive work.
Closing perspective
The most important insight here is not that diabetes technology works. It does.
The insight is that the hardest part of diabetes management is increasingly cognitive. Tools reduce uncertainty and improve perceived control, but the day still runs on interpretation and micro-decisions. When a condition never pauses, decision fatigue becomes the true burden.
The next phase will not be defined by better measurement alone. It will be defined by reliable decision offload that reduces attention demands, with fewer interruptions.
Frequently Asked Questions
Why can diabetes still feel exhausting even with CGM?
Because CGM reduces uncertainty, but daily decisions remain. Mental and emotional fatigue was the top burden at 51.5%.
Does CGM reduce stress?
For many, yes. 57.6% reported significantly reduced effort and stress, but decision-making load can persist.
What matters most in diabetes technology?
Accuracy and reliability at 39.4%, likely because reliable data reduces second-guessing.
Are predictive alerts helpful or overwhelming?
Most rate them helpful (60.6% very helpful), though helpfulness does not capture interruption burden.
What do people want technology to handle next?
Fewer decisions, especially the ones that repeat all day.
Hope this insight added value.
Participate in the survey below and add your voice to the conversation.
About Author : MDForlives
MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.


