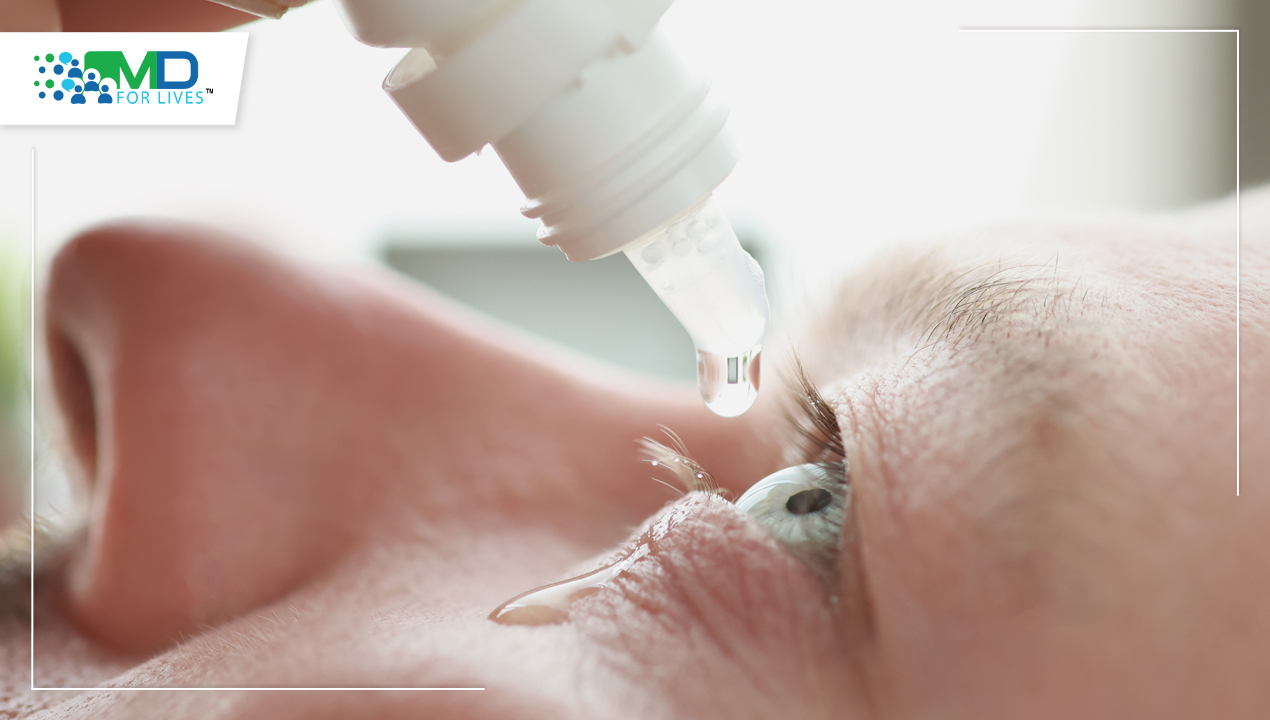
Cataract surgery is one of the most frequently performed ophthalmic procedures and remains the only definitive treatment for vision loss caused by cataracts. Cataracts develop when the eye’s natural lens becomes cloudy, leading to blurred vision, glare, reduced contrast sensitivity, and difficulty performing everyday tasks. While the surgical technique itself is highly standardized and safe, real-world outcomes are strongly influenced by how well patients understand the procedure, recovery expectations, and post-operative care requirements. This article explains how cataract surgery works, who typically needs it, what recovery involves, and why aftercare plays a critical role in patient satisfaction.
What Is Cataract Surgery?
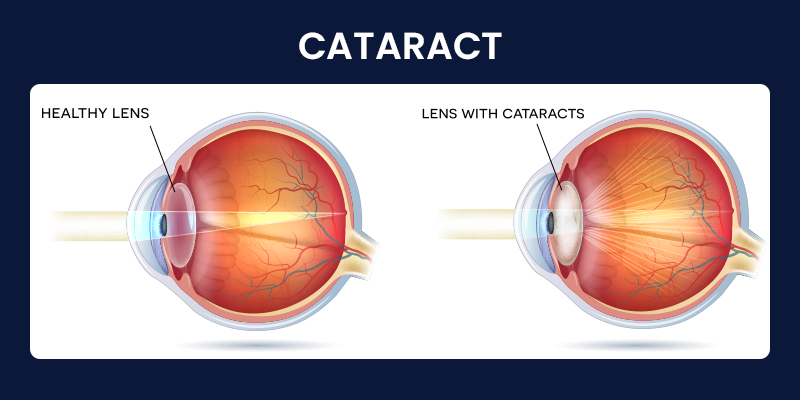
Cataract surgery is a minimally invasive procedure in which a cloudy natural lens is removed and replaced with a clear artificial lens called an intraocular lens (IOL). The objective is to restore visual clarity by allowing light to pass unobstructed through the eye and focus properly on the retina.
Cataracts cannot be reversed with medication or permanently corrected with glasses. Once they begin to interfere with daily activities, surgery is the only effective solution.
Why Is Cataract Surgery Done?
Cataract surgery is recommended when vision impairment begins to affect functional independence rather than at a specific clinical threshold alone. Common reasons include:
- Difficulty reading or seeing fine details
- Increased glare or halos around lights
- Reduced color perception
- Trouble driving, especially at night
- Frequent changes in spectacle prescriptions with limited improvement
From a clinical perspective, the decision to proceed with surgery is guided by both objective findings and patient-reported limitations. Many ophthalmologists note that quality-of-life impact often drives the timing of intervention more than visual acuity scores alone.
Who Needs Cataract Surgery?
Cataracts most commonly occur as part of the aging process, but they may also develop earlier due to:
- Diabetes and metabolic conditions
- Prolonged steroid use
- Excessive ultraviolet exposure
- Smoking
- Eye trauma or prior ocular surgery
- Genetic predisposition
Not every cataract requires immediate surgery. The decision is individualized and based on how much the cataract interferes with daily functioning and safety.
Cataract Tests Used for Diagnosis
A comprehensive eye evaluation is required to confirm cataracts and plan treatment.
Visual Acuity Test
Assesses clarity of vision at different distances.
Slit Lamp Examination
Allows detailed examination of the lens, cornea, and anterior eye structures.
Retinal Examination
Evaluates the retina and optic nerve to identify coexisting conditions that may influence surgical outcomes.
These tests also help determine the appropriate IOL type and power.
How Is Cataract Surgery Done?
Cataract surgery is typically performed as an outpatient procedure under local anesthesia.
Duration
The surgical procedure itself usually takes 15–20 minutes per eye, though total visit time is longer due to preparation and post-operative observation.
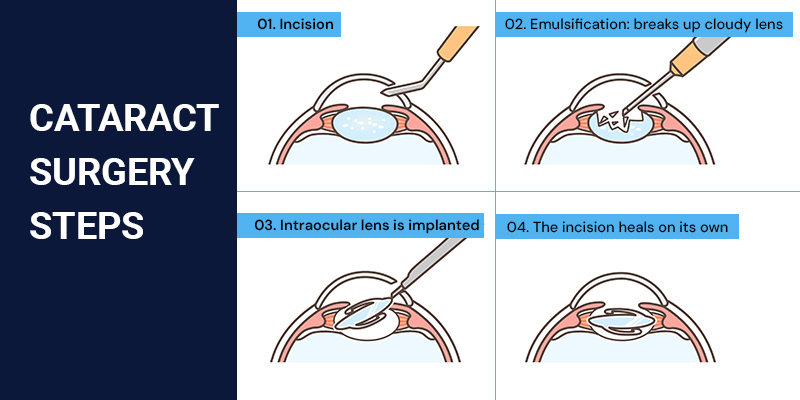
Procedure Overview
1. The eye is numbed using local anesthesia.
2. A small incision is made in the cornea.
3. Ultrasound energy is used to break the cloudy lens into fragments (phacoemulsification).
4. The fragments are removed.
5. A folded intraocular lens is inserted through the same incision.
6. The incision seals naturally in most cases.
Success Rate
It is widely regarded as highly successful. Most patients experience meaningful improvement in vision, provided there are no other underlying eye conditions, and post-operative instructions are followed closely.
What Happens During Cataract Surgery?
Patients remain awake but comfortable throughout the procedure. Pain is minimal, and most report only mild pressure or light sensitivity. Vision may appear bright or blurry during surgery, which is expected.
What Happens After Cataract Surgery?
Immediately after surgery, patients may notice blurred vision, watering, or mild irritation. These symptoms typically improve within the first few days.
Follow-up appointments are essential to:
- Monitor healing
- Adjust medications
- Identify early complications
Most ophthalmologists emphasize that recovery is gradual and varies between individuals.
Types of Cataract Surgery
Phacoemulsification
The most common technique, using ultrasound to remove the lens.
Laser-Assisted Cataract Surgery
Uses laser technology for specific surgical steps, offering added precision in selected cases.
Extracapsular Cataract Surgery
Used for advanced cataracts where the lens must be removed in one piece.
The choice of technique depends on cataract severity, ocular anatomy, and clinical judgment.
Benefits of Cataract Surgery
- Clearer, sharper vision
- Improved contrast and colour perception
- Reduced glare sensitivity
- Enhanced independence and daily functioning
While many patients reduce their dependence on glasses, outcomes vary based on IOL selection and individual visual needs.
What to Expect With Cataract Surgery
Setting realistic expectations is critical. While surgical success rates are high, vision may fluctuate during early recovery. Some patients expect immediate perfection, whereas clinicians often observe that satisfaction improves when patients understand the recovery timeline in advance.
Cataract Surgery Recovery
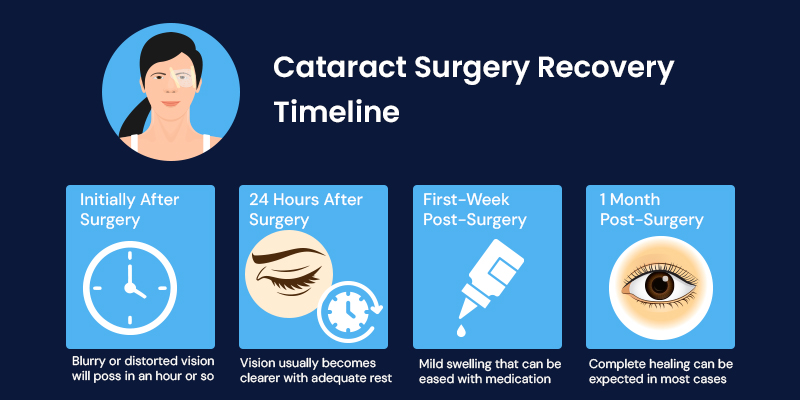
Recovery is generally smooth, but adherence to post-operative care significantly influences outcomes.
Recovery Timeline
- First 24–48 hours: Initial visual improvement, mild discomfort possible
- First week: Continued visual stabilization; light activities resume
- 2–4 weeks: Vision typically stabilizes
Activity Precautions
- Avoid rubbing the eye
- Avoid heavy lifting and strenuous activity initially
- Protect the eye from dust, water, and bright sunlight
- Use prescribed eye drops exactly as directed
Clinician Insight on Recovery Adherence
Ophthalmologists frequently observe that dissatisfaction following surgery is rarely due to the procedure itself. As one commonly expressed clinical observation notes:
“Patients often underestimate recovery discipline: it’s not the surgery, it’s the aftercare that determines satisfaction.”
This reflects a recurring pattern in real-world practice: patients who follow medication schedules and activity restrictions tend to report smoother recoveries and better visual outcomes.
What Are the Risks of Cataract Surgery?
Although surgery is considered very safe, potential risks include:
- Infection
- Inflammation
- Temporary increase in eye pressure
- Retinal detachment (rare)
- Posterior Capsular Opacification (PCO), a common delayed issue that can be treated with a simple laser procedure
Early detection through follow-up visits helps manage most complications effectively.
Cataract Surgery Costs
The cost of cataract surgery varies based on:
- Surgical technique
- Type of intraocular lens
- Geographic location
- Insurance or healthcare coverage
Standard surgery is often covered under many healthcare plans, while premium lens options may involve additional costs.
Nutrition and Diet After Cataract Surgery
Nutrition supports healing and overall eye health.
Foods to Include
- Leafy greens and colourful vegetables
- Citrus fruits rich in vitamin C
- Nuts and seeds containing vitamin E
- Fatty fish and plant-based omega-3 sources
- Lean proteins for tissue repair
Foods to Limit
- Excess sugar and highly processed foods
- High-sodium items
- Alcohol during early recovery
- Adequate hydration and balanced meals contribute to smoother recovery.
Cataract Surgery Recovery and Outlook
Most patients report significant improvements in vision and daily functioning after surgery. Long-term outcomes are generally stable, especially when recovery guidelines are followed and follow-up care is maintained.
Conclusion
Cataract surgery is a highly effective intervention for restoring vision and improving quality of life. While the procedure itself is standardized and safe, real-world outcomes depend heavily on patient understanding, expectation-setting, and adherence to post-operative care. Clear communication between patients and clinicians remains essential to achieving optimal results.
Frequently Asked Questions
How safe are cataract operations?
It is considered one of the safest surgical procedures. When performed by trained ophthalmologists and followed by proper post-operative care, serious complications are uncommon.
How long does cataract surgery take?
The surgical procedure usually takes about 15–20 minutes per eye, although total clinic time may be longer due to preparation and post-surgery observation.
How long does it take to recover from cataract surgery?
Initial recovery typically occurs within a few days. Most patients experience stable vision within 2 to 4 weeks, depending on individual healing and adherence to aftercare instructions.
Is cataract surgery painful?
It is generally painless. Local anesthesia is used, and patients may feel mild pressure or light sensitivity during the procedure.
What are the risks or complications of cataract surgery?
Possible risks include infection, inflammation, temporary vision disturbances, and posterior capsular opacification. Most complications are treatable when detected early through follow-up visits.
When can I drive after cataract surgery?
Many patients can resume driving within a few days after surgery, once their ophthalmologist confirms that vision meets safety requirements.
Is cataract surgery covered by insurance or Medicare?
Basic surgery is often covered by insurance or government healthcare programs, while premium intraocular lenses or advanced techniques may involve additional costs.

MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.