Immunotherapy has transformed cancer care by harnessing the immune system to target malignant cells. By improving survival outcomes across multiple cancer types, immune checkpoint inhibitors and related therapies have become integral to modern oncology practice. However, activating the immune system systemically also introduces unique side-effect profiles that differ from traditional chemotherapy.
Among these effects, ocular and visual complications are uncommon but clinically meaningful. While often overshadowed by more frequent immune-related adverse events, eye-related side effects of immunotherapy can affect quality of life, interfere with daily functioning, and complicate ongoing cancer treatment if not recognized early.
Understanding how and why these effects occur, what symptoms may signal early involvement, and how they are managed in real-world oncology practice is essential for both clinicians and patients.
How Immunotherapy Affects the Body?
Immunotherapy works by enhancing immune recognition of cancer cells. Drugs such as immune checkpoint inhibitors block regulatory pathways that normally limit immune activation, allowing T cells to mount a stronger anti-tumor response.
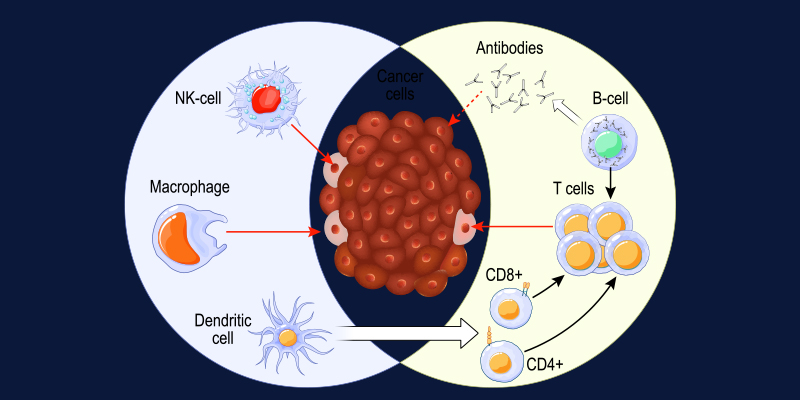
This immune amplification is not tumor-specific. As a result, healthy tissues may become unintended targets, leading to immune-related adverse events (irAEs). These effects can involve the skin, gastrointestinal tract, endocrine system, lungs, nervous system, and less commonly, the eyes.
Importantly, immune-related side effects may emerge weeks or months after treatment initiation, and in some cases, after initial treatment cycles are complete. This delayed presentation contributes to under-recognition in routine care.
Why Eye-Related Side Effects Matter?
Ocular side effects are relatively rare compared to other immunotherapy-related toxicities, but their impact can be disproportionate. Vision changes, eye discomfort, or inflammation can significantly affect a patient’s independence, ability to work, and overall well-being.
In routine oncology practice, eye-related symptoms may be subtle at onset and easily attributed to fatigue, aging, or unrelated eye conditions. Because patients may not proactively report mild visual changes unless prompted, ocular immune effects are sometimes identified later than other toxicities.
Early recognition allows for timely intervention and, in many cases, symptom resolution without requiring permanent discontinuation of cancer therapy.
Common Eye-Related Side Effects of Immunotherapy
Reported ocular immune-related adverse events include:
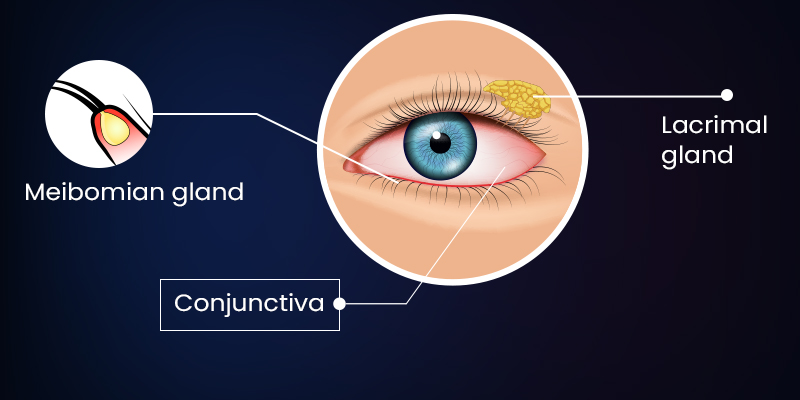
- Dry eye and ocular surface inflammation
Patients may experience irritation, redness, or a gritty sensation due to immune-mediated tear film disruption.
- Uveitis
Inflammation of the uveal tract can cause eye pain, redness, light sensitivity, and blurred vision.
- Optic neuritis
In rare cases, immune activation affects the optic nerve, leading to vision loss or changes in color perception.
- Retinal inflammation
Retinal involvement may present with floaters, visual distortion, or decreased visual acuity.
While these effects are uncommon, their clinical significance lies in the potential for vision impairment if diagnosis or treatment is delayed.
Why Ocular Side Effects May Be Missed?
Several factors contribute to delayed recognition of eye-related immunotherapy effects:
- Symptoms may be mild or intermittent initially
- Patients may not associate visual changes with cancer treatment
- Routine oncology visits often prioritize systemic symptoms
- Eye complaints may fall outside the typical oncology assessment framework
Because ocular effects can progress even when systemic symptoms are stable, proactive questioning about vision and eye comfort can play an important role in early detection.
Management and Monitoring in Clinical Practice
Management of immunotherapy-related ocular side effects typically involves collaboration between oncology and ophthalmology. Treatment approaches depend on severity and may include:
- Topical or systemic corticosteroids
- Temporary interruption of immunotherapy in moderate to severe cases
- Ongoing ophthalmologic monitoring
In many instances, symptoms improve with appropriate intervention, and cancer treatment can be safely resumed. The goal is not reflexive discontinuation, but balanced risk management that preserves both cancer control and visual function.
Patient Awareness and Communication
For patients receiving immunotherapy, understanding potential side effects supports earlier reporting and timely care. Patients should be encouraged to mention:
- New or worsening vision changes
- Eye pain, redness, or sensitivity to light
- Persistent dryness or irritation
Clear communication helps distinguish benign eye issues from immune-mediated effects that require evaluation.
Supporting Real-World Understanding of Immunotherapy Effects
Clinical trials establish safety profiles, but real-world care reveals how side effects present, evolve, and affect daily life. Platforms such as MDForLives support this understanding by capturing clinicians and patient experiences that reflect how immunotherapy is used beyond controlled research settings.
By complementing biomedical evidence with real-world observation, healthcare systems can better anticipate where side effects emerge and how they impact long-term care.
Conclusion
Immunotherapy has reshaped cancer treatment, offering meaningful benefits across many malignancies. While ocular side effects are uncommon, they represent an important aspect of immune-related toxicity that warrants attention.
Recognizing subtle symptoms, maintaining vigilance beyond early treatment cycles, and fostering collaboration across specialties can help prevent avoidable vision-related complications. As immunotherapy continues to expand across oncology, understanding its full spectrum of effects remains central to delivering high-quality, patient-centered care.
Frequently Asked Questions (FAQs)
Can immunotherapy affect the eyes?
Yes. Immunotherapy can cause eye-related side effects, although these are less common than other immune-related adverse events. When they occur, they are usually linked to immune-mediated inflammation affecting structures of the eye.
What kind of eye problems can occur with immunotherapy?
Reported eye-related side effects include dry eye symptoms, inflammation of the eye (such as uveitis), optic nerve inflammation, and, less commonly, retinal involvement. Symptoms may include redness, pain, blurred vision, light sensitivity, or visual disturbances.
Are eye side effects from immunotherapy common?
Eye-related side effects are considered uncommon compared to skin, gastrointestinal, or endocrine effects. However, their impact can be significant if not identified and managed early.
Why are eye-related side effects sometimes missed?
Eye symptoms may begin subtly and may not be immediately associated with cancer treatment. Patients may not report mild visual changes unless specifically asked, and oncology visits often focus on systemic symptoms rather than vision-related concerns.
When do eye side effects usually appear during immunotherapy?
Eye-related immune effects can occur at different points during treatment. In some cases, symptoms may develop weeks or months after therapy begins, or even after initial treatment cycles have been completed.
Should patients on immunotherapy see an eye specialist?
Routine eye exams are not required for all patients on immunotherapy. However, patients who develop new or worsening eye symptoms should be referred for ophthalmologic evaluation to determine whether symptoms may be treatment-related.
How are immunotherapy-related eye side effects treated?
Management depends on severity and may include topical treatments, systemic medications such as corticosteroids, or temporary adjustments to cancer therapy. Care is typically coordinated between oncology and ophthalmology teams.
Do eye side effects mean immunotherapy must be stopped?
Not always. Many eye-related side effects can be managed effectively without permanently discontinuing immunotherapy. Treatment decisions are individualized based on symptom severity, response to therapy, and overall cancer management goals.
What should patients report to their care team?
Patients should inform their healthcare team about any new vision changes, eye pain, redness, dryness, light sensitivity, or visual disturbances, even if symptoms seem mild or intermittent.
Why is monitoring eye symptoms important during immunotherapy?
Early recognition of eye-related side effects allows for timely intervention, which can help prevent complications and preserve vision while supporting the continuation of effective cancer treatment.

MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.



2 Comments
Cancer Imaging: Is Patients Reaping the Rewards? - MDforLives
5 years ago[…] unable to keep pace with the ever-growing number of increasingly sophisticated targeted agents and immunotherapies. The recent explosion in novel cancer imaging techniques should, therefore, provide much-needed […]
Advancements in Cancer Imaging: Are Patients Reaping the Rewards? - MDForLives
5 years ago[…] unable to keep pace with the ever-growing number of increasingly sophisticated targeted agents and immunotherapies. The recent explosion in novel cancer imaging techniques should, therefore, provide much-needed […]