Breast cancer recurrence remains a critical concern for survivors, with clinical evidence showing that relapse can occur months or even years after initial treatment. Understanding recurrence patterns, symptoms, and prevention strategies is essential for long-term disease management and improved outcomes.
What Is Breast Cancer Recurrence
Breast cancer recurrence refers to the return of cancer after initial treatment and a period of remission. It occurs when residual cancer cells survive therapy and later proliferate. Recurrence can happen locally, regionally, or at distant sites, depending on disease progression.
Types of Breast Cancer Recurrence
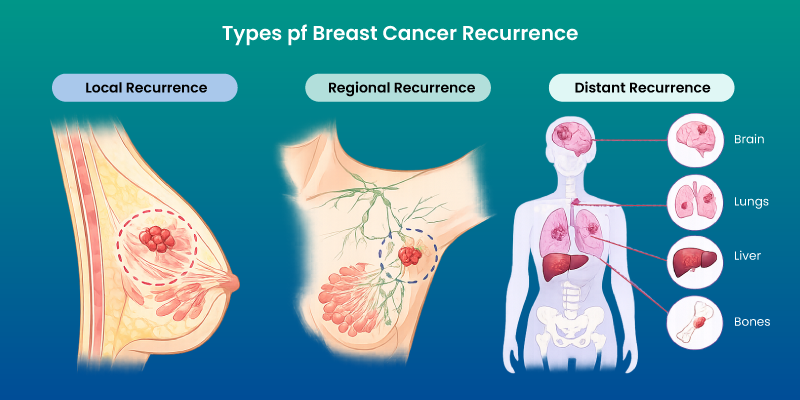
- Local recurrence
- Occurs in the same breast or surgical scar area.
- Regional recurrence
- Appears in nearby lymph nodes, such as underarm or chest nodes.
- Distant recurrence (metastatic)
Cancer spreads to organs such as bones, liver, lungs, or brain.
Breast Cancer Recurrence Rates
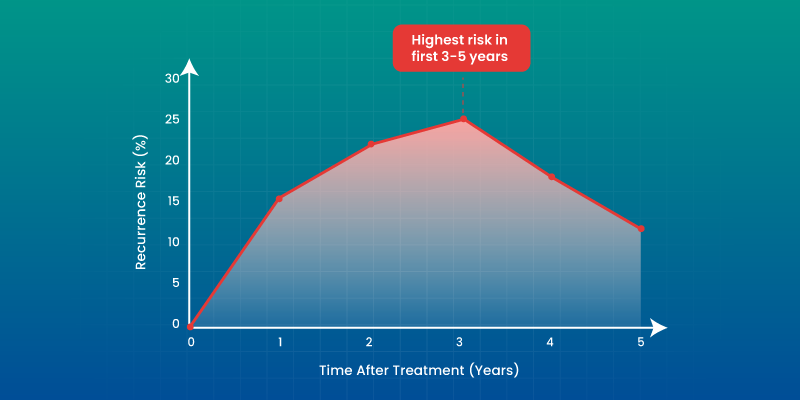
Breast cancer relapse statistics vary based on stage, tumor biology, and treatment approach.
- Early-stage cancers show lower recurrence rates, with stage 1 recurrence rates typically under 10% over 5 years.
- Hormone receptor-negative and HER2-positive cancers tend to have higher recurrence risks without targeted therapy.
- The highest recurrence risk is generally observed within the first 3 to 5 years post-treatment.
Understanding what type of breast cancer has the highest recurrence rate is essential. Triple-negative breast cancer is associated with higher early recurrence compared to hormone receptor-positive subtypes.
Symptoms of Breast Cancer Recurrence
Recognizing breast cancer recurrence symptoms early enables timely intervention.
Common symptoms include:
- New lump in breast or chest area
- Changes in breast shape or skin texture
- Persistent bone pain
- Shortness of breath
- Unexplained weight loss
- Fatigue or neurological symptoms in advanced cases
Symptoms vary depending on recurrence location, making regular follow-up critical.

Risk Factors for Breast Cancer Recurrence
Several clinical and lifestyle factors influence recurrence risk:
- Tumor size and stage at diagnosis
- Lymph node involvement
- Hormone receptor status
- Incomplete treatment adherence
- Genetic mutations such as BRCA1/2
- Obesity and physical inactivity
These variables are central to predicting breast cancer relapse probability.
Read also on Risk of Physical Inactivity
Diagnosis of Recurrent Breast Cancer
Diagnosis involves a combination of imaging and laboratory assessments:
- Mammography, MRI, or CT scans
- PET scans for metastatic detection
- Biopsy to confirm recurrence
- Blood markers in select cases
Clinical evaluation is tailored based on symptoms and previous cancer history.
Read also on PSMA PET Scan for Prostate Cancer
Treatment Options for Recurrent Breast Cancer
The treatment depends on recurrence type and prior therapies.
Common approaches include:
- Surgery for localized recurrence
- Radiation therapy if not previously administered
- Chemotherapy for systemic disease
- Hormone therapy for receptor-positive cancers
- Targeted therapies and immunotherapies
Emerging treatments such as targeted therapy and CAR-T approaches are expanding options for resistant cases.

Advances in Preventing Breast Cancer Recurrence
Recent studies highlight improvements in recurrence prevention:
- Extended hormone therapy beyond 5 years
- HER2-targeted therapies reducing relapse risk
- Personalized treatment guided by genomic profiling
- AI-driven monitoring for early detection
These advancements are shifting recurrence management from reactive to preventive.
Read also about Precision medicine
Lifestyle Changes That May Reduce Recurrence Risk
Evidence suggests that lifestyle plays a measurable role in recurrence reduction:
- Maintaining a healthy body weight
- Regular physical activity
- Limiting alcohol intake
- Balanced, nutrient-dense diet
- Stress management and sleep optimization
These interventions complement clinical treatments and improve long-term outcomes.
Read to know Does Alcohol Causes Cancer
Follow-Up Care for Breast Cancer Survivors
Structured follow-up protocols are critical:
- Regular clinical exams every 3 to 6 months initially
- Annual imaging based on risk profile
- Monitoring therapy adherence
- Managing long-term side effects
Follow-up care ensures early detection of recurrence and better prognosis.
Living With the Risk of Recurrence
Living with uncertainty is a documented challenge among survivors. Evidence indicates that patient education, peer support, and access to credible information improve psychological resilience and treatment adherence.
Conclusion
Breast cancer recurrence is a complex but manageable aspect of survivorship. With advancements in detection, targeted therapies, and preventive strategies, long-term outcomes continue to improve. A combination of clinical vigilance and informed lifestyle choices remains central to reducing recurrence risk.
Explore more evidence-led healthcare insights on global patient and clinician perspectives: MDForlives
Frequently Asked Questions
How many years after breast cancer can recurrence occur?
Recurrence can occur at any time, but risk is highest within the first 5 years. Hormone receptor-positive cancers may recur even after 10 years.
What are the early signs of breast cancer recurrence?
Early signs include new lumps, skin changes, persistent pain, or systemic symptoms such as fatigue and weight loss.
Does the stage of cancer affect breast cancer recurrence risk?
Yes, higher-stage cancers have a greater likelihood of recurrence due to increased tumor spread at diagnosis.

MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.