Psilocybin therapy is gaining attention as researchers explore new approaches to treating mental health conditions. Psilocybin, a naturally occurring psychedelic compound found in certain mushrooms, has been studied for its potential to support psychological healing when used in controlled therapeutic settings.
Unlike recreational use, psilocybin assisted therapy combines the compound with structured psychological support and clinical supervision. Early research suggests that this approach may help individuals with conditions such as depression, anxiety, and trauma-related disorders.
Interest in psilocybin mushroom therapy has increased significantly as scientists examine how psychedelic compounds interact with the brain and influence emotional processing.
What Is Psilocybin Therapy?
Psilocybin therapy is a form of mental health treatment that combines a psychedelic compound called psilocybin with guided psychological support.
Psilocybin is the active compound found in certain mushrooms commonly referred to as “magic mushrooms.” In therapeutic settings, the compound is administered under medical supervision as part of a structured treatment process.

The therapy typically includes three stages:
- Preparation sessions with therapists
- Controlled psilocybin experience
- Integration sessions where patients process insights from the experience
This structured model distinguishes psilocybin assisted therapy from unsupervised psychedelic use.
History of Psilocybin Research
Research into psilocybin mushroom therapy began in the 1950s when scientists started investigating the psychological effects of psychedelic substances.
Early studies explored the use of psychedelics in psychotherapy. However, research slowed significantly during the late 20th century due to regulatory restrictions.
In recent decades, renewed scientific interest has led to modern clinical studies examining the potential benefits of mushroom psychedelic therapy in treating mental health conditions.
Several academic institutions now conduct research into psilocybin’s therapeutic applications.
How Does Psilocybin Therapy Work?
Understanding how does psilocybin therapy work requires examining its effects on the brain.
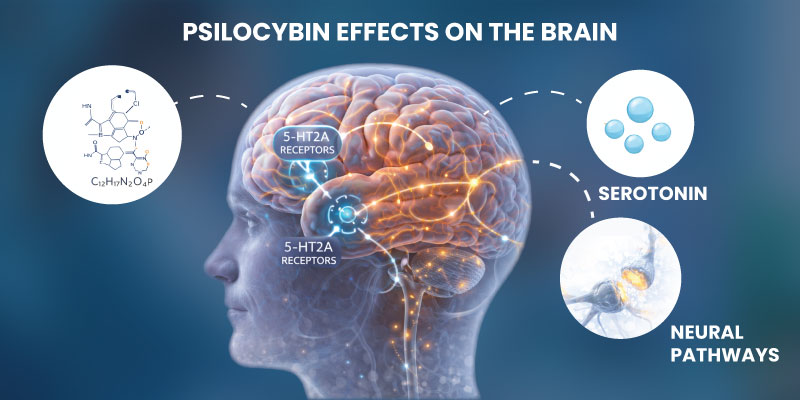
Psilocybin affects serotonin receptors, particularly the 5-HT2A receptor, which plays a role in mood, perception, and cognition.
Research suggests psilocybin may influence brain function in several ways:
Increased Brain Connectivity
Psilocybin appears to temporarily increase communication between different brain regions that do not usually interact.
Reduced Activity in the Default Mode Network
The default mode network is associated with self-focused thinking and rumination. Reduced activity in this network may help disrupt negative thought patterns.
Enhanced Emotional Processing
Psilocybin may allow patients to process emotional experiences from new perspectives.
These effects are believed to contribute to the therapeutic outcomes seen in psilocybin assisted therapy.
Psilocybin Therapy for Depression
One of the most widely studied applications is psilocybin therapy for depression.
Some clinical trials have explored its use in patients with treatment resistant depression who did not respond to conventional medications.
Early findings suggest that, when combined with psychotherapy, psilocybin may lead to improvements in depressive symptoms for some patients.
Researchers are studying whether these effects can be sustained over time and how treatment protocols can be optimized.
Benefits of Psilocybin Therapy
Several potential benefits of psilocybin therapy have been explored in clinical research.
Psychological Insight
Patients often report new perspectives on emotional experiences during therapy sessions.
Reduced Depression Symptoms
Some studies indicate improvements in mood and emotional well-being following treatment.
Improved Emotional Processing
Psilocybin therapy may help individuals process trauma or unresolved emotional challenges.
Enhanced Therapeutic Engagement
The experience may deepen engagement with psychotherapy sessions.
While these potential benefits are promising, more research is needed to confirm long-term outcomes.
Psilocybin Assisted Therapy Process
The structure of psilocybin assisted therapy is carefully designed to ensure safety and therapeutic value.
Preparation Phase
Before receiving psilocybin, patients meet with therapists to discuss expectations, emotional history, and treatment goals.
Preparation helps establish trust and psychological readiness.
Therapeutic Session
During the session, psilocybin is administered in a controlled environment under professional supervision.
Patients typically lie down in a calm setting while therapists monitor the experience.
Integration Phase
After the session, integration therapy helps patients process insights or emotions that emerged during the experience.
Integration sessions are considered essential for therapeutic benefit.
Safety Considerations in Psilocybin Therapy
Although research is promising, psilocybin therapy must be conducted under professional supervision.
Potential risks include:
- Anxiety or psychological distress during the experience
- Temporary confusion or altered perception
- Possible interactions with existing mental health conditions
Clinical protocols emphasize screening and medical oversight to reduce risk.
Read also about safety of ashwagandha
Legal and Regulatory Status
The legal status of psilocybin mushroom therapy varies across countries.
Some regions allow research studies or regulated therapeutic use, while others still classify psilocybin as a controlled substance.
In recent years, regulatory agencies have granted special research designations to support clinical trials exploring psilocybin therapy for depression and other mental health conditions.
Read also about Mental health in digital age
Psilocybin Therapy News and Research Developments
Recent psilocybin therapy news reflects growing interest in psychedelic medicine.
Research institutions and biotechnology companies are conducting clinical trials to evaluate:
- Treatment resistant depression
- Post-traumatic stress disorder
- Anxiety related to serious illness
- Substance use disorders
The expansion of clinical research may influence future regulatory decisions regarding mushroom psychedelic therapy.
Future of Psilocybin Therapy
The future of psilocybin therapy depends on ongoing research, regulatory approval, and clinical guidelines.
Scientists are investigating:
- Optimal dosing protocols
- Long term therapeutic effects
- Combination approaches with psychotherapy
- Safety profiles across different patient groups
If research continues to show positive outcomes, psilocybin assisted therapy may become part of mainstream mental health treatment in the future.
Key Takeaways
- Psilocybin therapy combines psychedelic compounds with structured psychological support.
- Research into psilocybin mushroom therapy is expanding rapidly.
- Early studies suggest potential benefits for depression and emotional processing.
- Therapy involves preparation, guided sessions, and integration therapy.
- Ongoing clinical research is shaping the future of psychedelic medicine.
Read also about sertraline antidepressant
Frequently Asked Questions
What is psilocybin therapy?
Psilocybin therapy is a treatment approach that combines the psychedelic compound psilocybin with guided psychological support to address mental health conditions.
How does psilocybin therapy work?
Psilocybin interacts with serotonin receptors in the brain, influencing mood, perception, and cognitive processing.
Is psilocybin therapy used for depression?
Clinical studies are exploring psilocybin therapy for depression, particularly for patients who do not respond to traditional treatments.
What are the benefits of psilocybin therapy?
Potential benefits include improved emotional processing, reduced depressive symptoms, and enhanced engagement with psychotherapy.

MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.





