Antimicrobial resistance is one of the most critical threats to global health, affecting the effectiveness of treatments for infections that were once easily manageable. As resistance increases, routine medical procedures and common infections carry higher risk, making early awareness and prevention essential.
What is Antimicrobial Resistance?
Antimicrobial resistance occurs when microorganisms such as bacteria, viruses, fungi, and parasites evolve in ways that reduce or eliminate the effectiveness of drugs designed to treat them.
This means infections become harder to treat, requiring stronger medications, longer treatment durations, or alternative therapies.
Read also about Antifungal Medications
Why Antimicrobial Resistance is a Global Health Threat
This issue extends beyond individual infections.
- Increased mortality from treatable infections
- Longer hospital stays
- Higher healthcare costs
- Reduced effectiveness of surgeries and cancer treatments
It is not limited to hospitals and affects communities worldwide.
Causes of Antimicrobial Resistance & Examples
Misuse of Antibiotics
Using antibiotics when not needed or stopping treatment early contributes to resistance. Read also about Antibiotics and Gut Health.
Overuse in Healthcare Settings
Frequent and unnecessary prescriptions increase selective pressure on microorganisms.
Agricultural Use
Antibiotics used in livestock can contribute to resistant strains that transfer to humans.
Poor Infection Control
Inadequate hygiene practices allow resistant organisms to spread.
Examples
- Methicillin-resistant Staphylococcus aureus (MRSA)
- Drug-resistant tuberculosis
- Multidrug-resistant gram-negative infections
How Antimicrobial Resistance Develops & Spreads
Microorganisms adapt through genetic changes.
- Mutations occur naturally
- Resistant strains survive treatment
- These strains multiply and spread
Transmission can occur through:
- Direct contact
- Contaminated surfaces
- Food and water systems
Types of Drug-Resistant Infections
| Type | Description |
| Multidrug-resistant | Resistant to multiple drugs |
| Extensively drug-resistant | Limited treatment options |
| Pan-resistant | Resistant to nearly all available drugs |
These categories reflect increasing levels of treatment difficulty.
Diagnosis & Detection of Antimicrobial Resistance
Accurate diagnosis is essential for effective treatment.
- Laboratory culture and sensitivity testing
- Molecular diagnostic techniques
- Surveillance systems
Early detection helps guide appropriate therapy.
Treatment Challenges in Antimicrobial Resistance
- Limited effective drug options
- Increased risk of treatment failure
- Need for combination therapies
- Higher cost and longer treatment duration
Developing new antimicrobials is complex and slow, making prevention critical.
Antimicrobial Stewardship
Stewardship programs aim to optimize the use of antimicrobial agents.
Key principles include:
- Prescribing only when necessary
- Choosing appropriate drug and dose
- Monitoring treatment outcomes
These programs reduce misuse and slow resistance development.
Prevention of Antimicrobial Resistance
For Individuals
- Avoid unnecessary antibiotic use
- Complete prescribed treatments
- Maintain hygiene and vaccination
For Healthcare Systems
- Implement infection control measures
- Promote responsible prescribing
- Strengthen surveillance systems
Role of Medical Professionals
Allied Health Professionals (AHP)
Support infection prevention, patient education, and adherence to treatment plans.
Pharmacists: How They Help Tackle Resistance
Pharmacists play a central role in managing antibiotic use.
- Review prescriptions for appropriateness
- Educate patients on correct use
- Support antibiotic stewardship programs
- Monitor adverse drug reactions
- Act as a bridge between patients and healthcare providers
Healthcare Providers (HCP)
Clinicians are responsible for accurate diagnosis, appropriate prescribing, and ongoing monitoring.
Emerging Solutions & Future Strategies
- Development of new antimicrobial agents
- Use of vaccines to reduce infection burden
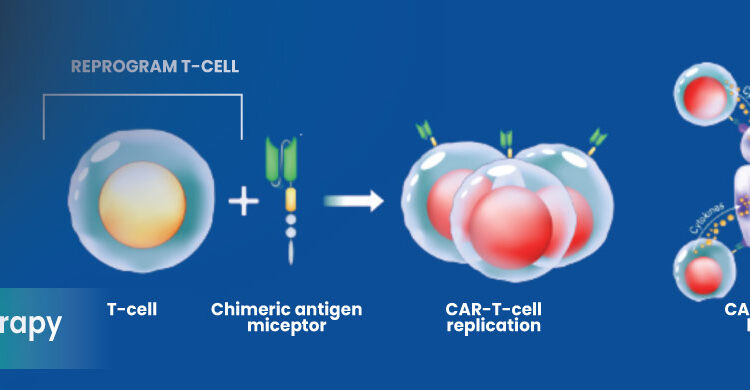
- Phage therapy and alternative treatments
- AI-driven surveillance and predictive models
These approaches aim to address both prevention and treatment challenges.
Conclusion
Antimicrobial resistance is a growing challenge that requires coordinated action across healthcare systems, communities, and policy frameworks. While treatment options are becoming limited, prevention, responsible use of antibiotics, and continued research remain key to managing this global threat.
Explore more healthcare insights
Frequently Asked Questions
How serious is antimicrobial resistance globally?
It is considered one of the leading global health threats, contributing to increased mortality and healthcare burden.
Can antimicrobial resistance be reversed?
Resistance cannot always be reversed, but its spread can be slowed through responsible antibiotic use and infection control.
Are there alternatives to antibiotics to avoid antimicrobial resistance?
Yes. Vaccines, phage therapy, and supportive care strategies are being explored as alternatives.
When should antibiotic therapy be initiated or withheld?
Antibiotics should only be used when there is clear evidence of bacterial infection, based on clinical evaluation and diagnostic testing.

MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.