Insulin pump and CGM are transforming how diabetes is managed by combining continuous insulin delivery with real-time glucose monitoring. This integration allows for more precise control, reduced manual intervention, and improved long-term outcomes. As diabetes care moves toward data-driven systems, these technologies are becoming central to modern insulin therapy.
What is an Insulin Pump and CGM?
Insulin pump and CGM are two distinct devices that serve complementary roles in diabetes management. While one delivers insulin, the other continuously tracks glucose levels, enabling more informed decisions.
What is an Insulin Pump?
An insulin pump is a small, wearable device that delivers insulin continuously through a catheter placed under the skin. It replaces multiple daily injections by providing:
- Basal insulin throughout the day
- Bolus doses during meals
This allows for more flexible and precise insulin delivery.
What is a Continuous Glucose Monitor (CGM)?
A CGM is a sensor-based device that tracks glucose levels in real time. It provides continuous data and alerts for high or low glucose levels.
Key functions include:
- Real-time glucose readings
- Trend analysis
- Alerts for fluctuations
This reduces the need for frequent finger-prick testing.
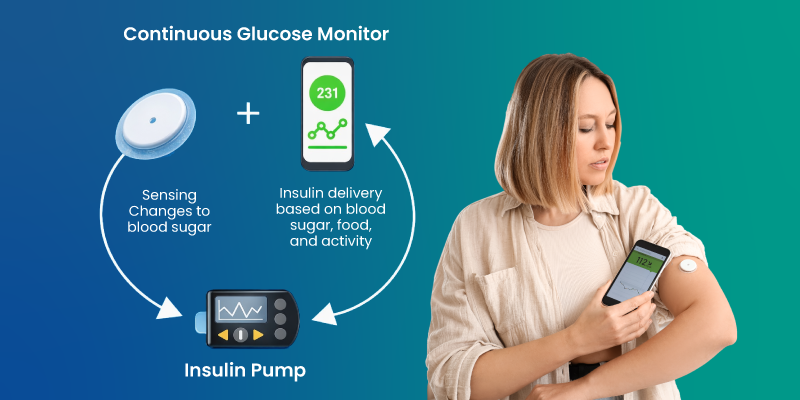
How Insulin Pump and CGM Work Together
When combined, these devices create a more responsive system.
- CGM tracks glucose levels continuously
- Data is transmitted to the pump or connected device
- Insulin delivery is adjusted based on trends
This interaction improves glycemic control and reduces variability. In advanced systems, the process becomes partially automated.
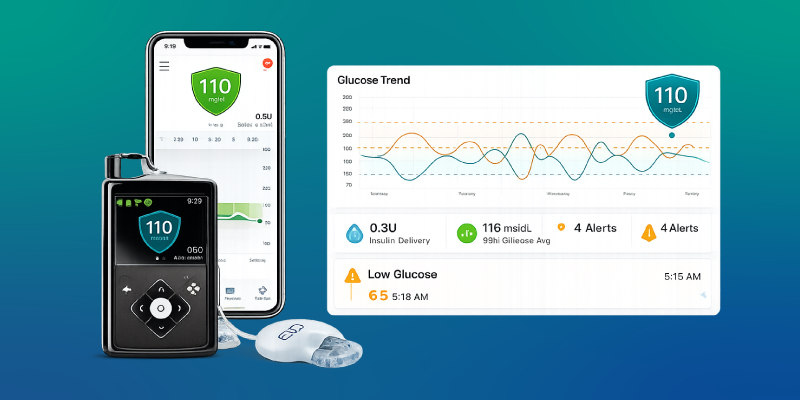
Types of Insulin Pump with CGM
Different levels of integration are available.
Standalone Devices
Pump and CGM operate separately but can be used together manually.
Integrated Systems
Devices communicate directly, allowing insulin adjustments based on glucose data.
Closed-Loop Systems
Also known as artificial pancreas systems, these automate insulin delivery based on continuous glucose input.
Benefits of Using Insulin Pump and CGM
Improved Glucose Control
Continuous monitoring and precise delivery reduce fluctuations.
Reduced Hypoglycemia Risk
Real-time alerts help prevent dangerous drops in glucose levels.
Greater Flexibility
Users can adjust insulin delivery based on lifestyle, meals, and activity.
Data-Driven Decisions
Trend insights enable better long-term management.
Risks and Limitations
- Device dependency and learning curve
- Cost and accessibility challenges
- Sensor inaccuracies in certain conditions
- Risk of technical malfunction
Understanding these limitations is essential before adoption.
Insulin Pump vs CGM: What is the Difference?
| Feature | Insulin Pump | CGM |
| Function | Delivers insulin | Monitors glucose |
| Role | Treatment | Monitoring |
| Data | Limited | Continuous |
| Automation | Possible with integration | Provides input for decisions |
Both devices serve different purposes but are most effective when used together.
Who Should Use Insulin Pump and CGM?
These technologies are suitable for:
- Individuals with type 1 diabetes
- Patients requiring intensive insulin therapy
- Those experiencing frequent glucose fluctuations
- Individuals seeking tighter glucose control
Clinical evaluation is required before use.
Read more about Healthy Living with Diabetes
Myth vs Reality: Insulin Pumps and CGMs
Myth: These devices eliminate the need for monitoring
Reality: Regular oversight and adjustments are still required
Myth: They work automatically without input
Reality: User interaction remains essential in most systems
Clinical Guidelines and Hospital Use
Healthcare providers recommend these technologies based on patient needs and clinical guidelines.
They are increasingly used in:
- Intensive diabetes management
- Pediatric diabetes care
- Long-term glycemic control strategies
Adoption is growing as evidence supports improved outcomes.
Real-Life Use: What Patients Experience
Patients often report:
- Reduced daily burden of injections
- Better awareness of glucose trends
- Increased confidence in managing diabetes
However, initial setup and adaptation require time and training.
Read real survey insights on whether Technology can make Diabetes Management Safer?
Insulin Pump and CGM: Advanced Technology
Closed-Loop System
Closed-loop systems automate insulin delivery based on real-time glucose data, reducing manual intervention.
Role of AI and Predictive Algorithms
Advanced systems use predictive models to anticipate glucose changes and adjust insulin delivery proactively.
This represents a shift toward automated diabetes management.
Training, Setup and Maintenance
Successful use depends on proper training.
- Device setup and calibration
- Understanding alerts and data trends
- Regular maintenance and sensor replacement
Ongoing education improves outcomes and user confidence.
Read also about How Cocoa Related to Diabetes
Conclusion
Insulin pump and CGM technologies are redefining diabetes management by combining continuous monitoring with precise insulin delivery. While they require initial effort and adaptation, their ability to improve control and reduce complications makes them a valuable option for many patients. As technology advances, these systems are expected to become even more integrated and automated.
Explore more healthcare insights: MDForLives
Frequently Asked Questions
Is an insulin pump better than injections?
It can provide more precise insulin delivery and flexibility, but suitability depends on individual needs.
Can an insulin pump control diabetes automatically?
Some advanced systems offer partial automation, but user input is still required.
Do you need a CGM if you have an insulin pump?
Not necessarily, but using both together improves monitoring and overall control.

MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.