Antifungal medications are essential for treating infections caused by fungi such as yeast, molds, and dermatophytes. These infections range from mild skin conditions to life-threatening systemic diseases, particularly in immunocompromised patients. Advances in antifungal pharmacology continue to improve treatment options while addressing emerging resistance and safety concerns.
Modern antifungal therapy focuses on targeted mechanisms that disrupt fungal cell membranes, cell walls, or metabolic pathways without harming human cells.
What Are Antifungal Medications?
Antifungal medications are drugs used to treat infections caused by fungi. They work by damaging fungal cell membranes, inhibiting cell wall synthesis, or interfering with fungal DNA production.
These medicines are used for conditions such as:
- skin and nail fungal infections
- yeast infections
- invasive fungal infections affecting organs or blood
Treatment may involve topical antifungal medications, oral antifungal drugs, or intravenous therapy depending on infection severity.
Classification and Overview of Antifungal Medications
Antifungal drugs are classified according to their chemical structure and mechanism of action.
| Drug Class | Example Drugs | Primary Target |
|---|---|---|
| Azoles | Fluconazole, Itraconazole | Ergosterol synthesis |
| Echinocandins | Caspofungin, Micafungin | Fungal cell wall |
| Polyenes | Amphotericin B | Cell membrane integrity |
| Allylamines | Terbinafine | Ergosterol production |
| Antimetabolites | Flucytosine | DNA synthesis |
These drug classes allow clinicians to select treatments based on infection type and fungal species.

Antifungal Drugs Mechanism of Action
The mechanism of action of antifungal drugs focuses on structures unique to fungal cells.
Common mechanisms include:
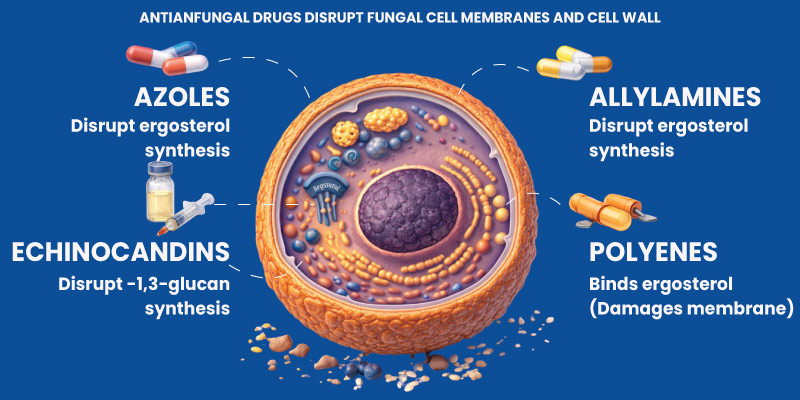
- Disruption of Cell Membranes: Polyenes bind to ergosterol in fungal cell membranes, causing leakage and cell death.
- Inhibition of Ergosterol Synthesis: Azole drugs block enzymes required to produce ergosterol, weakening fungal cell membranes.
- Inhibition of Cell Wall Formation: Echinocandins prevent synthesis of β-glucan, a key structural component of fungal cell walls.
- Interference With DNA and RNA Production: Antimetabolites disrupt fungal nucleic acid synthesis, preventing cell replication.
These mechanisms allow antifungal drugs to selectively target fungal pathogens.
Antifungals Pharmacokinetics, Drug Interactions and Safety
Pharmacokinetics influence how antifungal medications behave in the body.
Absorption: Some antifungal medications are available as oral antifungal drugs, while others require intravenous administration.
Drug Interactions: Azole antifungals frequently interact with other medications because they affect liver enzymes involved in drug metabolism.
Safety Considerations: Potential adverse effects include:
- liver toxicity
- kidney dysfunction
- gastrointestinal disturbances
Monitoring is especially important in patients receiving long-term therapy.
Antifungal Medicine Resistance
Resistance to antifungal drugs has become an increasing concern.
Mechanisms of resistance may include:
- genetic mutations in fungal targets
- increased drug efflux pumps
- reduced drug penetration into fungal cells
Emerging resistant organisms such as Candida auris highlight the need for improved diagnostics and new antifungal therapies.
Understanding resistance patterns helps clinicians choose appropriate treatments.
Clinical Applications of Antifungal Medications
Antifungal drugs are used in a wide range of infections.
Superficial Fungal Infections
These infections affect the skin, hair, or nails.
Examples include:
- athlete’s foot
- ringworm
- candidiasis
Treatment often involves topical antifungal medications.
Systemic Fungal Infections
Severe fungal infections may affect internal organs.
Examples include:
- invasive candidiasis
- aspergillosis
- cryptococcosis
These conditions usually require oral antifungal medications or intravenous therapy.
Common Antifungal Drugs Used in Clinical Practice
Some widely used antifungal medications include:
- Fluconazole for Candida infections
- Itraconazole for systemic fungal diseases
- Amphotericin B for severe invasive infections
- Terbinafine for fungal nail infections
- Caspofungin for resistant Candida infections
Selecting the correct antifungal medication depends on infection severity and pathogen type.
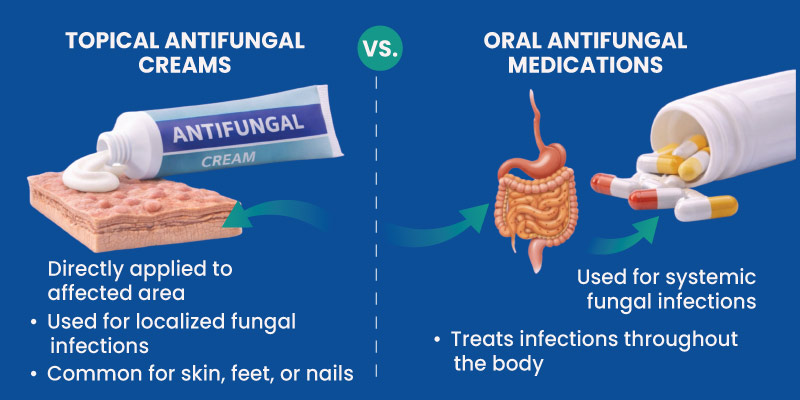
Topical vs Oral Antifungal Medications
Antifungal treatments may be delivered through different routes.
- Topical Antifungal Drugs: Topical antifungals include creams, sprays, and ointments used for skin infections.
- Oral Antifungal Medications: Oral antifungals are used for deeper or systemic infections that topical treatments cannot reach.
Choosing the appropriate treatment route depends on infection location and severity.
Antifungal Stewardship and Clinical Governance
Antifungal stewardship programs help ensure responsible antifungal use.
These programs aim to:
- improve diagnostic accuracy
- reduce unnecessary antifungal prescriptions
- limit drug resistance
- enhance treatment outcomes
Hospitals often implement multidisciplinary antifungal management strategies to improve patient care.
Antifungal Medications in Special Populations
Certain groups require additional caution when prescribing antifungal drugs.
- Immunocompromised Patients: Individuals undergoing chemotherapy or organ transplantation face higher risk of invasive fungal infections.
- Pediatric Patients: Children may require adjusted dosing based on age and metabolism.
- Pregnant Patients: Some antifungal drugs are contraindicated during pregnancy and require careful medical evaluation.
Challenges in Antifungal Therapy
Several challenges complicate antifungal treatment.
These include:
- limited drug classes
- increasing antifungal resistance
- delayed diagnosis of fungal infections
- potential drug toxicity
Improving diagnostic methods and developing new antifungal compounds remain important research priorities.
Read also about AI in Drug Discovery
Future Prospects in Antifungal Medicine Research
Ongoing research aims to develop safer and more effective antifungal therapies.
Areas of investigation include:
- discovery of new antifungal drug targets
- development of safer antifungal compounds
- improved molecular diagnostics
- understanding fungal pathogenic mechanisms
Researchers are studying fungal proteins and cellular pathways that could become targets for next-generation antifungal medications.
Key Takeaways
- Antifungal medications treat infections caused by fungi.
- Major drug classes include azoles, echinocandins, polyenes, and allylamines.
- Mechanisms of action target fungal cell membranes or cell wall synthesis.
- Resistance and drug interactions remain important clinical concerns.
- Ongoing research aims to develop safer antifungal treatments.
Read also about Antibiotics and gut health
Conclusion
Antifungal medications remain a cornerstone of modern infectious disease management. They treat conditions ranging from mild skin infections to severe systemic fungal diseases.
Understanding antifungal drug classes, mechanisms of action, resistance patterns, and clinical applications helps clinicians provide effective treatment. Continued research will be essential to address emerging resistance and expand therapeutic options.
Read also about Precision medicine
Frequently Asked Questions
When should echinocandins be used instead of azoles?
Echinocandins are often preferred for invasive Candida infections, particularly in critically ill patients or when azole resistance is suspected.
How do clinicians manage suspected antifungal resistance?
Laboratory testing and antifungal susceptibility testing help determine which antifungal medications remain effective.
How can drug interactions with azole antifungals be managed safely?
Doctors review patient medications carefully and monitor liver function because azoles affect enzymes involved in drug metabolism.
What determines the duration of antifungal therapy?
Treatment duration depends on infection type, severity, immune status, and clinical response.
Should combination antifungal therapy be used routinely?
Combination therapy may be used in severe or resistant infections but is not required for most routine fungal infections.

MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.