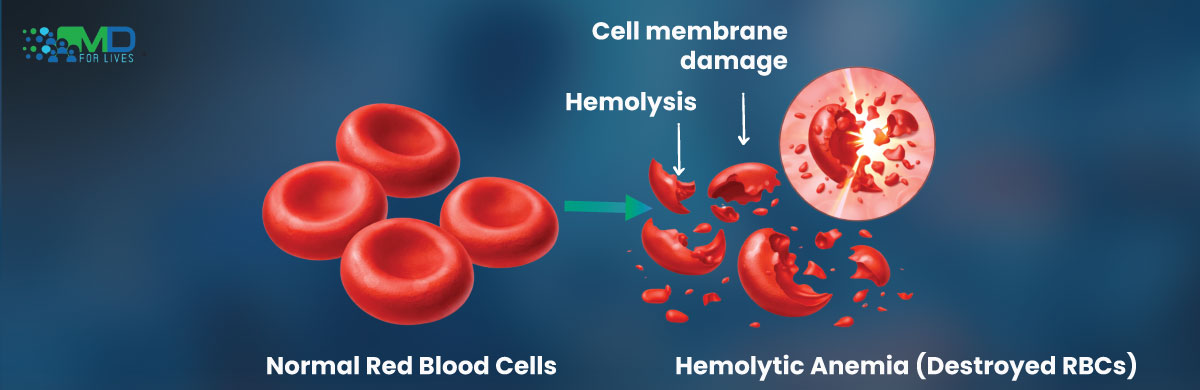
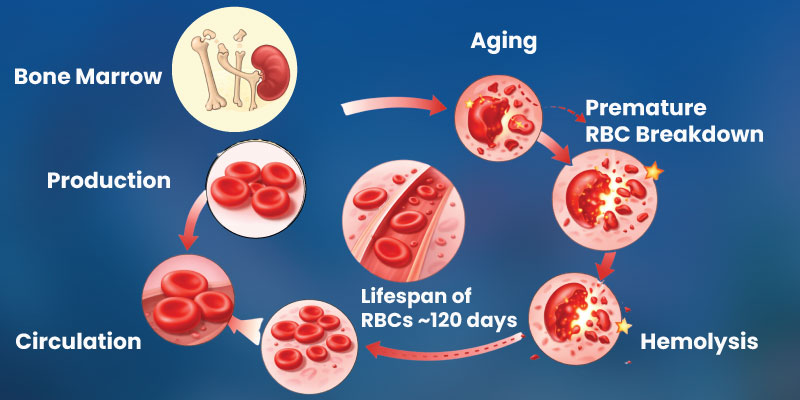
Hemolytic anemia is a condition in which red blood cells are destroyed faster than the body can replace them. Normally, these cells circulate in the bloodstream for about 120 days before being naturally removed and replaced.
When this process speeds up, the body cannot produce enough new red blood cells to maintain normal levels. The result is reduced oxygen delivery throughout the body, which may cause fatigue, shortness of breath, and other health concerns.
Understanding the symptoms, causes, diagnosis, and treatment options for this condition is important for early detection and proper management.
What Is Hemolytic Anemia?
To understand this disorder, it helps to look at the role of red blood cells.
Red blood cells carry oxygen from the lungs to tissues throughout the body and transport carbon dioxide back to the lungs for removal. When these cells break down prematurely, the body struggles to replace them quickly enough.
This imbalance leads to anemia caused by accelerated destruction of red blood cells, a process known as hemolysis.
The condition can be classified into two main types:
Inherited forms
These are caused by genetic conditions that affect red blood cell structure or function.
Acquired forms
These develop due to external factors such as immune reactions, infections, medications, or exposure to toxins.
Both types reduce the lifespan of red blood cells and limit oxygen delivery to tissues.
Symptoms of Hemolytic Anemia
Symptoms can vary depending on how quickly red blood cells are destroyed and the severity of the condition.
Common signs include:
- Fatigue or weakness
- Shortness of breath
- Pale or yellowish skin (jaundice)
- Rapid heart rate
- Dizziness or lightheadedness
- Dark colored urine
- Enlarged spleen

These symptoms occur because the body is attempting to compensate for the reduced number of circulating red blood cells.
In more severe cases, individuals may experience:
- Chest pain
- Extreme fatigue
- Rapid breathing
- Confusion
Sudden or severe symptoms require prompt medical evaluation.
Causes of Hemolytic Anemia
The destruction of red blood cells can occur for several reasons. Identifying the underlying cause is essential for determining the most appropriate treatment.
Genetic Causes
Some individuals inherit conditions that make red blood cells more fragile or abnormal.
Examples include:
- Sickle cell disease
- Thalassemia
- Hereditary spherocytosis
- Glucose 6 phosphate dehydrogenase deficiency (G6PD deficiency)
These disorders affect the shape, structure, or protective enzymes within red blood cells, making them more likely to break down prematurely.
Acquired Causes
In acquired forms, external factors trigger the destruction of otherwise healthy red blood cells.
Common causes include:
- Autoimmune diseases
- Certain infections
- Medication related immune reactions
- Exposure to toxins
- Mechanical damage to red blood cells
Among these, autoimmune hemolytic anemia occurs when the immune system mistakenly attacks red blood cells.
What Is the Most Common Cause?
The most common cause depends on whether the condition is inherited or acquired.
In adults, autoimmune hemolytic anemia is one of the most frequent acquired causes. The immune system produces antibodies that attach to red blood cells and lead to their destruction.
Globally, inherited conditions such as sickle cell disease and thalassemia are also major contributors.
How Doctors Diagnose the Condition
Diagnosis usually begins with a medical history, physical examination, and laboratory testing.
Common tests include:
- Complete blood count (CBC)
- Reticulocyte count
- Peripheral blood smear
- Lactate dehydrogenase (LDH) levels
- Bilirubin levels
- Haptoglobin levels

These tests help determine whether red blood cells are being destroyed faster than normal.
Additional testing may include:
- Coombs test to detect immune related hemolysis
- Genetic testing for inherited disorders
- Bone marrow examination in complex cases
Early diagnosis helps prevent complications and guides treatment decisions.
Treatment for Hemolytic Anemia
Treatment depends on the cause, severity of symptoms, and overall health of the patient. The goal is to reduce red blood cell destruction and support healthy blood production.
Medications
Doctors may prescribe medications to control immune activity or inflammation.
Common therapies include:
- Corticosteroids
- Immunosuppressive drugs
- Intravenous immunoglobulin (IVIG)
These treatments are often used when the immune system is responsible for destroying red blood cells.
Blood Transfusions
In severe cases, transfusions may be required to restore healthy red blood cell levels and improve oxygen delivery.
Transfusions are typically used when anemia becomes life threatening or causes significant symptoms.
Treating the Underlying Cause
If the disorder is triggered by infection, medication, or another health condition, treatment focuses on addressing the underlying factor.
Examples include:
- Discontinuing a triggering medication
- Treating infections
- Managing autoimmune disease
Surgical Treatment
Some patients with chronic forms may benefit from splenectomy, a surgical procedure that removes the spleen.
Because the spleen removes damaged red blood cells from circulation, removing it can reduce excessive cell destruction in certain cases.
Life Expectancy in Autoimmune Hemolytic Anemia
Many patients diagnosed with autoimmune hemolytic anemia respond well to treatment and maintain a good quality of life.
Life expectancy depends on several factors, including the underlying cause, severity of the condition, and response to therapy.
Early diagnosis, appropriate treatment, and regular monitoring significantly improve long term outcomes.
Complications of Hemolytic Anemia
If untreated, the disorder can lead to several complications.
Potential complications include:
- Severe anemia
- Gallstones due to increased bilirubin levels
- Enlarged spleen
- Heart related complications caused by chronic anemia
Appropriate treatment and medical monitoring help reduce these risks.
Living With the Hemolytic Anemia Condition
Many people manage this disorder successfully with appropriate medical care and lifestyle adjustments.
Helpful strategies include:
- Attending regular medical checkups
- Monitoring symptoms and blood test results
- Maintaining balanced nutrition
- Avoiding medications or triggers known to cause red blood cell destruction
Close communication with healthcare providers supports effective long term management.
When to See a Doctor
Medical evaluation is recommended if someone experiences:
- Persistent fatigue
- Yellowing of the skin or eyes
- Dark urine
- Unexplained weakness or dizziness
Early diagnosis helps determine whether red blood cell destruction or another medical condition is responsible for the symptoms.
Conclusion
Hemolytic anemia is a condition characterized by the premature destruction of red blood cells. Understanding its symptoms, causes, diagnostic methods, and treatment options helps patients and healthcare providers identify the disorder early and manage it effectively.
Advances in medical research continue to improve treatment strategies and patient outcomes. With proper care and monitoring, many individuals can maintain active and healthy lives.
Read also eating disorders and weight loss
Frequently Asked Questions
What is the most common cause of hemolytic anemia?
The most common acquired cause is autoimmune hemolytic anemia, where the immune system mistakenly attacks red blood cells. Globally, inherited conditions such as sickle cell disease and thalassemia are also frequent causes of hemolysis.
How is hemolytic anemia diagnosed?
Doctors diagnose hemolytic anemia using blood tests such as complete blood count, reticulocyte count, bilirubin levels, LDH levels, and haptoglobin levels. A Coombs test may be used to determine whether the immune system is destroying red blood cells.
What is autoimmune hemolytic anemia life expectancy?
Life expectancy varies depending on severity and response to treatment. Many people with autoimmune hemolytic anemia live normal lives when the condition is diagnosed early and managed with medications, monitoring, and treatment of underlying causes.
What are the warning signs of hemolytic anemia?
Early warning signs include persistent fatigue, pale skin, jaundice, dark urine, shortness of breath, and dizziness. These symptoms occur because the body does not have enough red blood cells to carry oxygen effectively.
Can hemolytic anemia be prevented?
Inherited forms cannot be prevented, but some acquired forms may be reduced by avoiding triggering medications, treating infections early, and managing autoimmune conditions under medical supervision.

MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.