Robotic surgery is transforming modern operating rooms by enhancing precision, control, and visualization in complex procedures. As robotic assisted surgery becomes more widely adopted across specialties, the conversation is shifting from innovation alone to evidence, outcomes, and ethical considerations.
Understanding how robotic surgery works, where it adds value, and where limitations remain is essential for both clinicians and healthcare systems.
Why & How Robotic Surgery Matters Today
It addresses key limitations of traditional open and laparoscopic approaches.
Key drivers of adoption include:
- need for minimally invasive procedures
- demand for faster recovery
- improved surgical precision
- enhanced visualization through 3D imaging
Robotic systems allow surgeons to operate with greater dexterity and control, especially in confined anatomical spaces.
Evolution of Robotic Surgery
Key Milestones in Surgical Robotics
- Early robotic systems introduced for basic assistance
- Development of the da Vinci Surgical System, enabling complex procedures
- Expansion into multiple specialties including urology and cardiothoracic surgery
- Integration with imaging and digital platforms
The evolution reflects a shift from mechanical assistance to intelligent surgical systems.
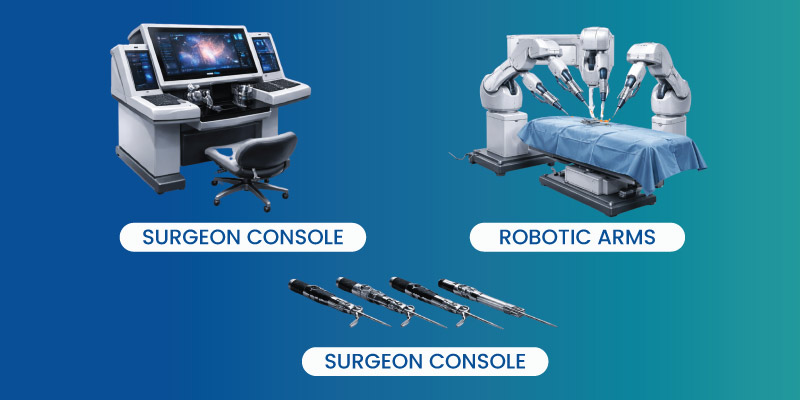
Types of Robotic Surgical Equipment and Systems
The Da Vinci Surgical System
The most widely used system, offering high-definition 3D visualization and precise instrument control.
Versius Minimally Invasive Robotic System
Designed for flexibility and modular deployment in operating rooms.
The Corindus CorPath GRX
Primarily used in vascular and cardiac interventions.
The Hugo RAS Robotic System
A newer platform focused on accessibility and scalability.
ZEUS Robotic Surgical System
An earlier system that contributed to the development of modern robotic platforms.
Advantages and Disadvantages of Robotic Surgery
Advantages of Robotic Surgery
- enhanced precision and control
- smaller incisions and reduced scarring
- shorter hospital stays
- improved visualization for surgeons
- reduced blood loss in many procedures
Disadvantages of Robotic Surgery
- high cost of equipment and procedures
- steep learning curve
- dependence on technology
- limited availability in some regions
The balance between benefits and limitations depends on clinical context.
Clinical Applications Across Specialties
Urology and Robotic Prostatectomy
One of the most common uses, offering precision in delicate anatomical structures.
Gynecology and Reproductive Surgery
Used for procedures such as hysterectomy and endometriosis treatment.
General and Colorectal Surgery
Applied in minimally invasive bowel surgeries.
Cardiothoracic and Thoracic Procedures
Used in heart and lung surgeries requiring precision.
Head and Neck and Oncological Surgery
Supports tumor removal with minimal damage to surrounding tissue.

Robotic Surgery Uses in Urology & Beyond
It is widely used in:
- prostate cancer surgery
- kidney procedures
- bladder surgeries
Its application continues to expand into other specialties as technology evolves.
Evidence-Based Outcomes and Clinical Effectiveness
Perioperative Outcomes and Recovery
Studies show:
- reduced hospital stays
- faster recovery times
- lower complication rates in selected procedures
Oncological and Long-Term Results
In cancer surgeries, robotic approaches may offer comparable outcomes to traditional methods.
Comparative Studies: Robotics vs Laparoscopy vs Open Surgery
Evidence suggests:
- robotic surgery improves precision
- laparoscopic surgery remains cost-effective
- open surgery may still be necessary in complex cases
Current Controversies in Evidence
Not all studies show clear superiority. Cost-effectiveness and outcome variability remain areas of debate.
Ethical, Legal, and Regulatory Perspectives
Transparency in Patient Communication
Patients should be informed about risks, benefits, and alternatives.
Surgeons remain responsible for outcomes, even when using robotic systems.
Device Safety and Liability
Hospitals and manufacturers share responsibility for system safety.
Data Privacy and Digital Health Concerns
Robotic systems often integrate with digital platforms, raising data security considerations.
Robotic Surgery Challenges, Limitations, and Practical Barriers
Technical and Mechanical Limitations
System malfunctions, though rare, can occur.
Infrastructure and Setup Constraints
High setup costs limit accessibility in many healthcare settings.
Overutilization and Appropriateness of Use
Not all procedures require robotic assistance.
Dependence on Industry Support
Ongoing maintenance and updates rely on manufacturers.

Future Directions and Innovations in Robotic Surgery
Artificial Intelligence and Decision Support
AI may assist with surgical planning and intraoperative guidance.
Haptic Feedback and Sensory Technology
Future systems may restore tactile sensation for surgeons.
Telesurgery and Remote Collaboration
Remote procedures may expand access to specialized care.
Towards Semi-Autonomous Surgery
Research is exploring systems that can assist with specific surgical tasks.
Real-World Experiences and Clinical Insights
Common Pitfalls for Beginners
- over-reliance on the system
- difficulty adapting to console-based surgery
Optimizing Outcomes in Early Practice
Training and simulation improve proficiency.
Case-Based Reflections
Early adoption highlights the importance of structured learning and team coordination.
Policy, Guidelines, and Institutional Governance
National and International Society Guidelines
Professional bodies provide frameworks for safe robotic surgery practice.
Hospital Accreditation Standards
Institutions must meet safety and training requirements.
Quality Assurance and Audit Systems
Regular audits help maintain clinical standards.
Continuing Medical Education
Ongoing training ensures skill development and patient safety.
Conclusion
Robotic surgery represents a significant advancement in modern medicine, offering precision, improved visualization, and minimally invasive options across multiple specialties.
However, its value lies not only in innovation but in appropriate use, clinical evidence, and ethical practice. As technology evolves, balancing access, cost, and outcomes will define the future of robotic assisted surgery.
Frequently Asked Questions
Is formal certification mandatory for performing robotic surgery?
Yes. Most institutions require specialized training and certification before surgeons can perform robotic procedures.
Is robotic surgery safe?
Robotic surgery is generally safe when performed by trained professionals, though outcomes depend on procedure type and expertise.
Is robotic surgery clinically superior to laparoscopy or open surgery?
It offers advantages in precision and visualization, but superiority depends on the specific procedure.
Who is responsible if technical errors occur during surgery?
The operating surgeon holds primary responsibility, supported by institutional and manufacturer accountability.
How long does it take to become proficient in robotic surgery?
Proficiency varies but typically requires structured training and experience over multiple procedures.

MDForLives is a global healthcare intelligence platform where real-world perspectives are transformed into validated insights. We bring together diverse healthcare experiences to discover, share, and shape the future of healthcare through data-backed understanding.